What's in this article?
What is Typhus?
Typhus fevers are caused by the rickettsiae bacteria and transmitted by arthropod (e.g. flea, mite, tick) bites. When arthropods bite a victim, they leave the rickettsaie bacteria behind. Scratching the bite opens the skin to the bacteria, allowing them to enter the bloodstream. Within the blood stream, the bacteria grow and replicate.
Different arthropods carry specific rickettsaie bacteria for each type of typhus. Typhus symptoms vary slightly by type. The most common symptoms are universal, affecting nearly all typhus patients.
Treatment focuses on using antibiotic medication to stop the infection. Untreated typhus can lead to serious complications and be potentially fatal. Prevention of typhus is easier than treatment. Methods of prevention focus on destroying or avoiding arthropod infestations.
What are Typhus Symptoms and Signs?
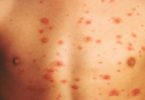
Symptoms of endemic typhus develop within about one to two weeks after initial infection and may include a high fever (about 105 F), headache, malaise, nausea, vomiting, diarrhea, and a rash that begins about four to seven days on the chest and abdomen after the initial symptoms above develop; the rash often spreads. Some patients may also have a cough and abdominal,joint, andback pain. Symptoms may last for about two weeks and, barring complications or death (less than 2% die), symptoms abate.
However, epidemic typhus symptoms, although initially similar to endemic typhus, become more severe. The rash may cover the entire body except the palms of the hands and the bottoms of the feet. Patients may develop additional symptoms of bleeding into the skin (petechiae), delirium, stupor, hypotension, and shock, which can cause their death.
Causes of Typhus
Typhus is caused by 2 types of bacteria: Rickettsia typhi or Rickettsia prowazekii.
Rickettsia typhi causes endemic or murine typhus.
- Endemic typhus is uncommon in the United States. It is usually seen in areas where hygiene is poor and the temperature is cold. Endemic typhus is sometimes called “jail fever.” The bacteria that causes this type is usually spread from rats to fleas to humans.
- Murine typhus occurs in the southern United States, particularly California and Texas. It is often seen during the summer and fall. It is rarely deadly. You are more likely to get this type of typhus if you are around rat feces or fleas, and other animals such as cats, possums, raccoons, and skunks.
Rickettsia prowazekii causes epidemic typhus. It is spread by lice.
Brill-Zinsser disease is a mild form of epidemic typhus. It occurs when the bacteria becomes active again in a person who was previously infected. It is more common in the elderly.
FACTS about Typhus
- Typhus is a bacterial disease; there are two types termed endemic and epidemic.
- Typhus has a long and deadly history, especially epidemic typhus.
- Typhus is caused by bacteria. Rickettsia prowazekii causes epidemic typhus. Rickettsia typhi and, occasionally, R. felis cause endemic typhus and are transmitted to humans by vectors such as lice (mainly epidemic) and fleas (mainly endemic).
- Risk factors include visiting or living in areas where rats, mice, and other animals have high populations (for example, disaster areas, poverty-stricken areas, refugee camps, jails) where vectors such as fleas and lice can carry the bacteria from the animals to infect humans.
- Endemic typhus symptoms can include rash that begins on the body trunk and spreads, high fever, nausea, malaise, diarrhea, and vomiting; Epidemic typhus has similar but more severe symptoms, including bleeding into the skin, delirium, hypotension, and death.
- Typhus is diagnosed by patient history, physical exam, and several tests (PCR, histological staining) based on immunological techniques. Some tests may need to be done in state or CDC labs.
- Antibiotics (for example, azithromycin [Zithromax, Zmax], doxycycline [Vibramycin, Oracea, Adoxa, Atridox], tetracycline [Sumycin], or chloramphenicol) are used to treat endemic and epidemic typhus.
- The prognosis for endemic typhus is usually good to excellent, but the epidemic typhus prognosis can range from good, with early effective treatment, to poor, with the elderly often having the worst prognosis.
- Both types of typhus can be reduced or prevented by good hygiene and clean living conditions that reduce or eliminate exposure to rats, mice, and other animals and the vectors that they carry (lice, fleas). There is no commercially available vaccine against either endemic or epidemic typhus.
How do you catch epidemic Typhus?
Epidemic typhus is passed from human to human by body lice. These are not the same as head lice or pubic lice, which are a nuisance, but don’t transmit disease.
The body lice become infected with Rickettsia prowazekii bacteria when they feed on the blood of an infected person.
If you catch these infected body lice (for example, by using a louse-infested blanket), their infected faeces will be deposited on your skin as they feed on your blood.
You only need to scratch a bite to rub the contaminated lice faeces into the tiny wound on your skin to become infected.
Less commonly, you can catch epidemic typhus by breathing infected dried body louse faeces in airborne dust.
Diagnosing Typhus
If you suspect that you have typhus, your doctor will ask about your symptoms and your medical history, including any travel or bites you may have received. To help with the diagnosis, tell your doctor if you:
- are living in a crowded environment
- know of a typhus outbreak in your community
- have a history of travel
Diagnosis is difficult because symptoms are common to other diseases, including:
- dengue (breakbone fever)
- malaria (infectious disease spread by mosquitos)
- brucellosis (infectious disease caused by the brucella bacteria)
Diagnostic tests for the presence of typhus include:
- Western blot (test to identify presence of typhus bacteria)
- immunofluorescence test (using fluorescent dyes to detect typhus in sputum samples)
- blood test (results can indicate the presence of infection)
Typhus Pictures