What's in this article?
- 1 Breast Cancer Today
- 2 Breast Cancer Symptoms
- 3 Signs of Inflammatory Breast Cancer
- 4 Breast Cancer and Mammograms
- 5 Breast Ultrasound and MRI
- 6 Breast Self-Exams
- 7 What If You Find a Lump?
- 8 Breast Biopsy
- 9 Hormone-Sensitive Breast Cancer
- 10 HER2-Positive Breast Cancer
- 11 Breast Cancer Stages
- 12 Breast Cancer Survival Rates
- 13 Breast Cancer Surgery
- 14 Radiation Therapy for Breast Cancer
- 15 Chemotherapy for Breast Cancer
- 16 Hormone Therapy for Breast Cancer
- 17 Targeted Drugs for Breast Cancer
- 18 Life After Diagnosis
- 19 Breast Reconstruction
- 20 Breast Forms
- 21 Breast Cancer: Why Me?
- 22 Breast Cancer Genes
- 23 Risk Factors in Your Control
- 24 Breast Cancer Research
Breast Cancer Today
Breast cancer today is not what it was 20 years ago. Survival rates are climbing, thanks to greater awareness, more early detection, and advances in treatment. For roughly 200,000 Americans who are diagnosed with breast cancer each year, there are plenty of reasons to be hopeful.
Breast Cancer Symptoms
There are often no symptoms of breast cancer, but sometimes women may discover a breast problem on their own. Signs and symptoms to be aware of may include:
- A painless lump in the breast.
- Changes in breast size or shape.
- Swelling in the armpit.
- Nipple changes or discharge.
Breast pain can also be a symptom of cancer, but this is not common.
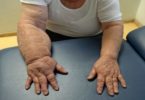
Signs of Inflammatory Breast Cancer
Inflammatory breast cancer is a rare, fast-growing type of cancer that often causes no distinct lump. Instead, breast skin may become thick, red, and may look pitted like an orange peel. The area may also feel warm or tender and have small bumps that look like a rash.
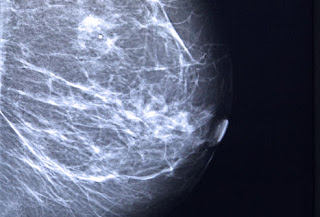
Breast Cancer and Mammograms
The earlier breast cancer is found, the easier it is to treat. And mammograms, X-rays of the breast, can detect tumors before they are large enough to feel. The American Cancer Society recommends yearly mammograms beginning at age 40 for women at average risk. While the U.S. Preventive Services Task Force recommends a screening mammogram every two years from age 50 to 74. It also notes that before age 50, each woman should check with a doctor to find out what screening schedule is right for her, considering the potential benefits and harms from screening.
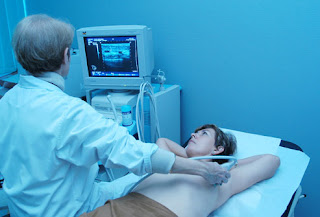
Breast Ultrasound and MRI
Besides a mammogram, your doctor may order additional imaging with breast ultrasound. An ultrasound can help determine the presence of cysts, fluid-filled sacs that are not cancer. An MRI may be recommended along with a mammogram for routine screening in certain women who have a higher risk of breast cancer.
Breast Self-Exams
It was once widely recommended that women check their own breasts once a month. But studies suggest these breast self-exams play a very small role in finding cancer. The current thinking is that it’s more important to know your breasts and be aware of any changes, rather than checking them on a regular schedule. If you want to do breast self-exams, be sure to go over the technique with your doctor.
What If You Find a Lump?
First, don’t panic. Eighty percent of breast lumps are not cancerous. Lumps often turn out to be harmless cysts or tissue changes related to your menstrual cycle. But you should let your doctor know right away if you find anything unusual in your breast. If it is cancer, the earlier it’s found the better. And if it’s not, testing can give you peace of mind.
Breast Biopsy
The only sure way to determine whether a lump is cancer is to do a biopsy. This involves taking a tissue sample for further examination in the lab, sometimes through a small needle. Sometimes surgery is done to take part of or the entire lump for testing. The results will show whether the lump is cancer, and if so, what type. There are several forms of breast cancer, and treatments are carefully matched to the type of cancer.
Hormone-Sensitive Breast Cancer
Some types of breast cancer are fueled by the hormones estrogen or progesterone. A biopsy can reveal whether a tumor has receptors for estrogen (ER-positive) and/or progesterone (PR-positive). About two out of three breast cancers are hormone sensitive. There are several medications that keep the hormones from promoting further cancer growth.
The image shows a molecular model of an estrogen receptor.
HER2-Positive Breast Cancer
In about 20% of patients, breast cancer cells have too many receptors for a protein called HER2. This type of cancer is known as HER2-positive, and it tends to spread faster than other forms of breast cancer. It’s important to determine whether a tumor is HER2-positive, because there are special treatments for this form of cancer.
A HER2-positive breast cancer cell is illustrated here, with abnormal growth signals shown in green.
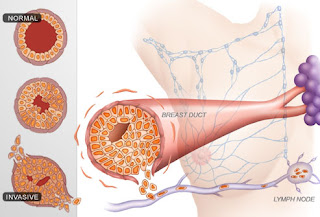
Breast Cancer Stages
Once breast cancer has been diagnosed, the next step is to determine how big the tumor is and how far the cancer has spread. This process is called staging. Doctors use Stages 0-4 to describe whether cancer is localized to the breast, has invaded nearby lymph nodes, or has spread to other organs, such as the lungs. Knowing the stage and type of breast cancer will help your health care team formulate a treatment strategy.
Breast Cancer Survival Rates
The odds of surviving breast cancer are strongly tied to how early it is found. According to the American Cancer Society, 100% of women with Stage 1 breast cancer live at least five years, compared to women without cancer – and many women in this group remain cancer-free for good. The more advanced the cancer, the lower this figure becomes. By Stage 4, the five-year relative survival rate declines to 20%. But these rates can improve as more effective treatments are found.
Breast Cancer Surgery
There are many types of breast cancer surgery, from taking out the area around the lump (lumpectomy or breast-conservation surgery) to removing the entire breast (mastectomy.) It’s best to discuss the pros and cons of each of these procedures with your doctor before deciding what’s right for you.
Radiation Therapy for Breast Cancer
Radiation therapy uses high-energy rays to kill cancer cells. It may be used after breast cancer surgery to wipe out any cancer cells that remain. It can also be used along with chemotherapy for treatment of cancer that has spread to other parts of the body. Side effects can include fatigue and swelling or a sunburn-like feeling in the treated area.
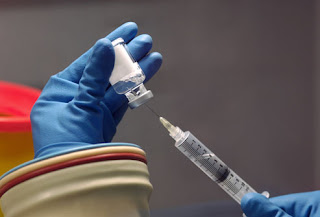
Chemotherapy for Breast Cancer
Chemotherapy uses drugs to kill cancer cells anywhere in the body. The drugs are often given by IV, but are sometimes taken by mouth or shot. Chemotherapy may be done after surgery to lower the odds of the cancer coming back. In women with advanced breast cancer, chemotherapy can help control the cancer’s growth. Side effects may include hair loss, nausea, fatigue, and a higher risk of infection.
Hormone Therapy for Breast Cancer
Hormone therapy is an effective treatment for women with ER-positive or PR-positive breast cancer. These are cancers that grow more rapidly in response to the hormones estrogen or progesterone. Hormone therapy can block this effect. It is most often used after breast cancer surgery to help keep the cancer from coming back. It may also be used to reduce the chance of breast cancer developing in women who are at high risk.
Targeted Drugs for Breast Cancer
Targeted therapies are newer drugs that target specific properties within cancer cells. For example, women with HER2-positive breast cancer have too much of a protein called HER2. Targeted therapies can stop this protein from promoting the growth of cancer cells. These drugs are often used in combination with chemotherapy. They tend to have milder side effects compared to chemotherapy.
Life After Diagnosis
There’s no doubt that cancer is a life-changing experience. The treatments can wear you out. You may have trouble managing daily chores, work, or social outings. This can lead to feelings of isolation. It’s crucial to reach out to friends and family for support. They may be able to go with you to treatments, help out with chores, or just remind you that you are not alone. Many people choose to join a support group — either locally or online.
Breast Reconstruction
Many women who have a breast removed choose to undergo reconstructive surgery. This replaces the skin, nipple, and breast tissue that are lost during a mastectomy. Reconstruction can be done with a breast implant or with tissue from somewhere else in your body, such as the tummy. Some women opt to begin reconstruction at the same time as their mastectomy. But it’s also possible to have reconstructive surgery months or years later.
Breast Forms
An alternative to breast reconstruction is to be fitted for a breast form. This is a breast-shaped prosthesis that fits inside your bra. Wearing a breast form allows you to have a balanced look when you are dressed — without undergoing additional surgery. Like reconstructive surgery, breast forms are often covered by insurance.
Breast Cancer: Why Me?
The most obvious risk factor for breast cancer is being a woman. Men get the disease, too, but it is about 100 times more common in women. Other top risk factors include being over age 55 or having a close relative who has had the disease. But keep in mind that up to 80% of women with breast cancer have no family history of the illness.
Breast Cancer Genes
Some women have a very high risk of breast cancer because they inherited changes in certain genes. The genes most commonly involved in breast cancer are known as BRCA1 and BRCA2. Women with mutations in these genes have up to an 80 percent chance of getting breast cancer at some point in life. Other genes may be linked to breast cancer risk as well.
Risk Factors in Your Control
Being overweight, getting too little exercise, and drinking more than one alcoholic beverage per day can raise the risk of developing breast cancer. Birth control pills and some forms of postmenopausal hormone therapy can also boost your risk. But the risk goes back to normal after these medications are stopped. Among survivors, good lifestyle choices may be helpful. Recent studies suggest that physical activity may help lower the risk of a recurrence and it’s a proven mood-booster.
Breast Cancer Research
Doctors continue to search for more effective and tolerable treatments for breast cancer. The funding for this research comes from many sources, including advocacy groups throughout the country. Many of the 2.5 million breast cancer survivors and their families choose to participate in walk-a-thons and other fundraising events. This links each individual fight against cancer into a common effort for progress.

























My spouse and I absolutely love your blog and
find most of your post's to be precisely what I'm looking for.
Would you offer guest writers to write content to suit your needs?
I wouldn't mind producing a post or elaborating on most of the subjects
you write concerning here. Again, awesome website!
Feel free to visit my site :: Idolize REviews
Inspiring quest there. What occurred after? Good luck!
my page; beauty tips
Nice post. I was checking continuously this blog and I am impressed!
Extremely helpful information specially the last part :)
I care for such information much. I was seeking this certain information for a long time.
Thank you and best of luck.
Feel free to surf to my blog; natural green coffee bean
Hi there! This article couldn't be written any better!
Looking through this article reminds me of my previous roommate!
He always kept preaching about this. I am going to forward this
information to him. Pretty sure he's going to have a very good
read. Many thanks for sharing!
Here is my site: trance
It's wonderful that you are getting thoughts from this piece of writing as well
as from our discussion made here.
My page anti age serum
Hello my family member! I want to say that this post
is amazing, nice written and include approximately all significant infos.
I'd like to peer extra posts like this .
My web-site … muscles to work out
I think the admin of this web page is actually working hard in favor
of his website, for the reason that here every data is quality based
material.
Here is my homepage … Nutra Green Coffee Cleanse