What's in this article?
Typhus: Introduction
Typhus: A general name for various arthropod-borne rickettsial infections.
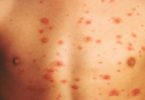
When infected arthropods bite someone, they may leave the bacteria that cause typhus behind. Scratching the bite opens the skin and allows the bacteria to enter the bloodstream. Once in the bloodstream, the bacteria reproduce and grow.
How is typhus diagnosed?
The diagnosis is based on the patient’s clinical history, physical exam, and tests based on identification of the bacterial genus and species by PCR testing of a skin biopsy from skin rash or lesions, or blood samples. Immunohistological staining can identify the bacteria within infected tissue (skin tissue, usually). Typhus can also be diagnosed, usually late or after the disease has been treated with antibiotics, when significant titers of anti-rickettsial antibodies are detected by immunological techniques. Although some state labs may do these tests, the CDC should be contacted for testing questions and be given information if there is an outbreak of epidemic typhus. These tests help distinguish between epidemic and endemic typhus, anthrax, and other viral diseases.
Diagnostic tests for the presence of typhus include:
- skin biopsy (sample of the skin from your rash will be tested in a lab)
- Western blot (test to identify presence of typhus bacteria)
- immunofluorescence test (using fluorescent dyes to detect typhus in samples of sputum, which is the thick fluid or mucus found in the lungs and the breathing passages)
- blood test (results can indicate the presence of infection)
Treatment for Typhus
Treatment includes antibiotics such as:
- Doxycycline
- Tetracycline
- Chloramphenicol (less common)
Tetracycline taken by mouth can permanently stain teeth that are still forming. It is usually not prescribed for children until after all of their permanent teeth have grown in.
Patients with epidemic typhus may need intravenous fluids and oxygen.