What's in this article?
What is Scleroderma?
Scleroderma affects women more often than men and most commonly occurs between the ages of 30 and 50. While there is no cure for scleroderma, a variety of treatments can ease symptoms and improve quality of life.
The word “scleroderma” comes from two Greek words: “sclero” meaning hard, and “derma” meaning skin. Hardening of the skin is one of the most visible manifestations of the disease. The disease has been called “progressive systemic sclerosis,” but the use of that term has been discouraged since it has been found that scleroderma is not necessarily progressive. The disease varies from patient to patient.
Causes of Scleroderma
The cause of scleroderma is not known. Researchers have found some evidence that certain genes are important hereditary factors, but the environment seems to also play a role. The result is activation of the immune system in a susceptible individual, causing damage to the inner lining of tiny blood vessels and injury to tissues that result in scar tissue formation and the accumulation of excess collagen.
The fact that genes seem to cause a predisposition to developing scleroderma means that inheritance at least plays a partial role. It is not unusual to find other autoimmune diseases in families of scleroderma patients. Some evidence for the role genes may play in leading to the development of scleroderma comes from the study of Choctaw Native Americans who are the group with the highest reported prevalence of the disease. The disease is more frequent in females than in males.
Symptoms of Scleroderma
The symptoms can affect many parts of your body. They include:
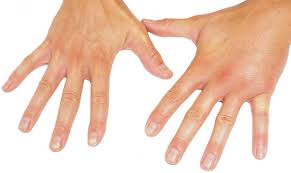
- Hardened or thickened skin that looks shiny and smooth. It’s most common on the hands and face.
- Cold fingers or toes that turn red, white, or blue. This is called Raynaud’s phenomenon.
- Ulcers or sores on fingertips
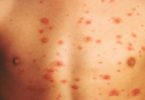
- Small red spots on the face and chest. These are opened blood vessels called telangiectasias.
- Puffy or swollen or painful fingers and/or toes
- Painful or swollen joints
- Muscle weakness
- Dry eyes or mouth (called Sjogren’s syndrome)
- Swelling mostly of the hands and fingers. Your doctor may call this edema.
- Shortness of breath
- Heartburn
- Diarrhea
- Weight Loss
How serious is Scleroderma?
Any chronic disease can be serious. The symptoms of scleroderma vary greatly for each person, and the effects of scleroderma can range from very mild to life threatening. The seriousness will depend on the parts of the body, which are affected, and the extent to which they are affected. A mild case can become more serious if not properly treated. Prompt and proper diagnosis and treatment by qualified physicians may minimize the symptoms of scleroderma and lessen the chance for irreversible damage.
Scleroderma Diagnosis
Because scleroderma can take so many forms and affect so many different areas of the body, it can be difficult to diagnose.
After a thorough physical exam, your doctor may suggest blood tests to check for elevated blood levels of certain antibodies produced by the immune system. He or she may remove a small tissue sample (biopsy) of your affected skin so that it can be examined in the laboratory for abnormalities.
Your doctor may also suggest breathing tests (pulmonary function tests), a CT scan of your lungs and an echocardiogram of your heart.
Treatments for Scleroderma
There’s no treatment for scleroderma, but you can manage the symptoms. Your doctor will focus on helping you do that with:
- NSAIDs (nonsteroidal anti-inflammatory drugs like ibuprofen or aspirin). They can help with swelling and pain.
- Steroids and other drugs to control your immune response. These can help with muscle, joint, or internal organ problems.
- Drugs that boost blood flow to your fingers
- Blood pressure medication
- Drugs that open blood vessels in the lungs or prevent tissue from scarring
- Heartburn medication
Other things that help may include:
- Exercise for better overall health
- Skin treatment, including light and laser therapy
- Physical therapy
- Occupational therapy
- Stress management
- If severe organ damage happens, organ transplantation

Leave a Comment