What's in this article?
What is Atopic Dermatitis?
Atopic dermatitis is a common, often long-lasting skin disease that affects a large percentage of the world’s population. Atopy is a special type of hypersensitivity that is associated with asthma, inhalant allergies (hay fever), and a chronic dermatitis. There is a known hereditary component of the disease, and it is more common in affected families. Criteria that enable a doctor to diagnose it include the typical appearance and distribution of the rash in a patient with a personal or family history of asthma and/or hay fever.
The term atopic is from the Greek meaning “strange.” The term dermatitis means inflammation of the skin.
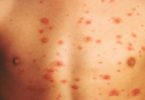
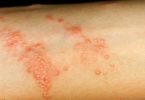
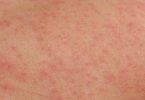
In atopic dermatitis, the skin becomes extremely itchy and inflamed, causing redness, swelling, vesicle formation (minute blisters), cracking, weeping, crusting, and scaling. This type of eruption is termed eczematous. In addition, dry skin is a very common complaint in almost all those afflicted with atopic dermatitis.
Although atopic dermatitis can occur in any age, most often it affects infants and young children. Occasionally, it may persist into adulthood or may actually appear at that time. Some patients tend to have a protracted course with ups and downs. In most cases, there are periods of time when the disease is worse, called exacerbations or flares, which are followed by periods when the skin improves or clears up entirely, called remissions. Many children with atopic dermatitis enter into a permanent remission of the disease when they get older, although their skin may remain somewhat dry and easily irritated.
Multiple factors can trigger or worsen atopic dermatitis, including low humidity, seasonal allergies, exposure to harsh soaps and detergents, and cold weather. Environmental factors can activate symptoms of atopic dermatitis at any time in the lives of individuals who have inherited the atopic disease trait.
Causes Atopic Dermatitis?
The cause of atopic dermatitis isn’t clear, but it affects your skin’s ability to hold moisture. Your skin becomes dry, itchy, and easily irritated.
Most people who have atopic dermatitis have a personal or family history of allergies, such as hay fever (allergic rhinitis) or asthma.
Things that may make atopic dermatitis worse include:
- Allergens, such as dust mites or animal dander.
- Harsh soaps or detergents.
- Weather changes, especially dry and cold.
- Stress.
- An allergic reaction to certain foods, such as eggs, peanuts, milk, wheat, fish, or soy products.
- Skin infection.
Symptoms of Atopic Dermatitis
Atopic dermatitis (eczema) signs and symptoms vary widely from person to person and include:
- Itching, which may be severe, especially at night
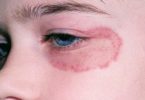
- Red to brownish-gray patches, especially on the hands, feet, ankles, wrists, neck, upper chest, eyelids, inside the bend of the elbows and knees, and, in infants, the face and scalp
- Small, raised bumps, which may leak fluid and crust over when scratched
- Thickened, cracked, dry, scaly skin
- Raw, sensitive, swollen skin from scratching
Atopic dermatitis most often begins before age 5 and may persist into adolescence and adulthood. For some people, it flares periodically and then clears up for a time, even for several years.
Treatment for Atopic Dermatitis
Treatment cannot cure AD, but it can control AD. Treatment is important because it can:
- Prevent the AD from getting worse.
- Calm the skin, relieving pain and itch.
- Reduce emotional stress.
- Prevent infections.
- Stop the skin from thickening. Thickened skin often itches all the time — even when the AD is not flaring.
A treatment plan often includes medicine, skin care, and lifestyle changes. Skin care and lifestyle changes can help prevent flare-ups. Many patients receive tips for coping. Doing all of this may seem bothersome, but sticking to the plan can make a big difference.
A dermatologist will create a treatment plan tailored to the patient’s needs. Medicine and other therapies will be prescribed as needed to:
- Control itching.
- Reduce skin inflammation (redness and swelling).
- Clear infection.
- Loosen and remove scaly lesions.
- Reduce new lesions from forming.
Home Treatment for Atopic Dermatitis
Home treatment for atopic dermatitis includes taking care of your skin and avoiding things that irritate it.
Take care of your skin
- Keep your skin hydrated through bathing in warm (not hot) water and applying moisturizer right afterwards.
Atopic Dermatitis: Taking Care of Your Skin
- Avoid things that irritate a rash or make it worse, such as soaps that dry the skin, perfumes, and scratchy clothing or bedding.
- Avoid possible allergens that cause a rash or make a rash worse, such as dust mites, animal dander, and certain foods.
Control itching and scratching
- Keep your fingernails trimmed and filed smooth to help prevent damaging the skin when you scratch it.
- Use protective dressings to keep from rubbing the affected area. Put mittens or cotton socks on your baby’s hands to help prevent him or her from scratching the area.
- Try coal tar preparations. When applied to the skin, they may help reduce itching. But if your itching gets worse after using coal tar, stop using it.
Avoid sun and stress
- Exposure to natural sunlight can be helpful for atopic dermatitis, but it is important to avoid sunburn. Too much sun, sweating, and/or getting too hot also can irritate the skin. When you use a sunscreen, choose one for sensitive skin.
- Reduce stress to help your skin and keep rashes from getting worse. Try relaxation techniques, behavior modification, or biofeedback. Massage therapy is also helpful, especially in children.


Leave a Comment