What's in this article?
According to the National Cancer Institute, there are about 56,000 new cases of thyroid cancer in the US each year, and the majority of those diagnoses are papillary thyroid cancer the most common type of thyroid cancer. Females are more likely to have thyroid cancer at a ratio of 3:1. Thyroid cancer can occur in any age group, although it is most common after age 30, and its aggressiveness increases significantly in older patients. Thyroid cancer does not always cause symptoms; often, the first sign of thyroid cancer is a thyroid nodule.
Causes of Thyroid cancer
It’s not clear what causes thyroid cancer.
Thyroid cancer occurs when cells in your thyroid undergo genetic changes (mutations). The mutations allow the cells to grow and multiply rapidly. The cells also lose the ability to die, as normal cells would. The accumulating abnormal thyroid cells form a tumor. The abnormal cells can invade nearby tissue and can spread throughout the body.
Types of thyroid cancer
The type of thyroid cancer you have determines treatment and prognosis. Types of thyroid cancer include:
- Papillary thyroid cancer. The most common form of thyroid cancer, papillary cancer arises from follicular cells, which produce and store thyroid hormones. Papillary thyroid cancer can occur at any age, but most often it affects people ages 30-50.
- Follicular thyroid cancer. Follicular cancer also arises from the follicular cells of the thyroid. It usually affects people older than age 50. Hurthle cell cancer is a rare and potentially more aggressive type of follicular thyroid cancer.
- Medullary thyroid cancer. Medullary thyroid cancer begins in thyroid cells called C cells that produce the hormone calcitonin. Elevated levels of calcitonin in the blood can detect medullary thyroid cancer at a very early stage. Certain genetic syndromes increase the risk of medullary thyroid cancer, although this genetic link is uncommon.
- Anaplastic thyroid cancer. Anaplastic thyroid cancer is a rare and rapidly growing cancer that is very difficult to treat. Anaplastic thyroid cancer typically occurs in adults age 60 or older.
- Thyroid lymphoma. Thyroid lymphoma is a rare form of thyroid cancer that begins in the immune system cells in the thyroid and grows very quickly. Thyroid lymphoma typically occurs in older adults.
Symptoms of thyroid cancer
In its early stages, thyroid cancer tends to cause no or very few symptoms.
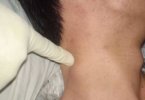
The main symptom of thyroid cancer is a lump or swelling at the front of the neck just below your Adam’s apple, which is usually painless.
Women also have Adam’s apples, but they’re much smaller and less prominent than a man’s.
The lymph nodes in your neck can also be affected and become swollen. Lymph nodes are small glands that are part of the lymphatic system, which helps fight infection.
Other symptoms of thyroid cancer only tend to occur after the condition has reached an advanced stage, and may include:
- unexplained hoarseness that doesn’t get better after a few weeks
- a sore throat or difficulty swallowing that doesn’t get better
- pain in your neck
How is thyroid cancer diagnosed?
Once a lump in the thyroid is discovered, it is important to know whether it is benign or malignant (cancerous).
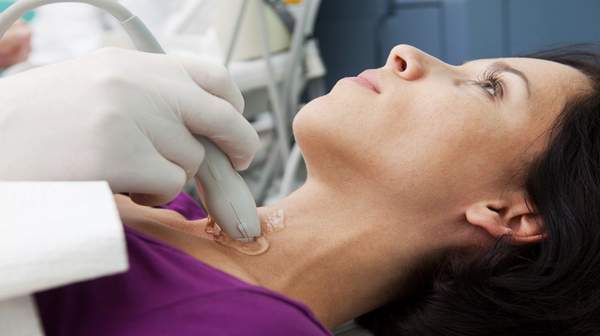
Often an ultrasound is performed to assess whether there is a single nodule or multiple nodules are present. Ultrasound can determine whether the nodule is fluid filled or solid. Ultrasound also can determine the general appearance of thyroid looking for inflammation or irregularities and the presence of enlarged lymph nodes nearby that may represent metastatic cancer.
Fine needle aspiration biopsy is the procedure performed to obtain a sample of cells from the nodule to determine if it is cancerous. Using ultrasound, a thin needle is placed into the nodule and cells from the nodule are obtained. These cells can be examined under a microscope by a pathologist to determine whether a cancer is present and if so, what type of cancer it is.
Results of the aspiration are usually reported as the following:
- Malignant: risk of malignancy is 100%
- Suspicious for malignancy: risk of malignancy is 50% to 75%
- Follicular cancer: risk of malignancy is 20% to 30%
- Atypical cells of unknown significance: risk of malignancy is 5% to 10%
- Benign: risk of malignancy is less than 1%
Sometimes, the results of the aspiration are unclear and indeterminate, and the aspiration may need to be repeated to get a better sample and more cells to study.
Another test involves ingesting radioactive iodine, which is taken up by the thyroid gland. The gland is scanned by a Geiger counter-type of apparatus that determines how much radioactive iodine has been taken up by the gland and any thyroid nodules. If the nodule picks up much of the iodine, it is referred to as a “hot nodule.” Such nodules are rarely cancerous. Nodules that take up little to no iodine are referred to as “cold nodules.” Although the overwhelming majority of such nodules are benign, 5% turn out to be malignant. Although thyroid scans may be helpful, aspiration of the gland is a much more useful test.
Blood tests may be ordered to determine thyroid hormone levels and levels of other hormones and electrolytes, like calcium, within the body. These tests indicate whether the cells of the thyroid produce too much or too little hormone, not if cancer is present.
On occasion CT, MRI, or PET scans may be useful in evaluating the neck structures if there is concern that thyroid cancer has spread (metastasized).
How is thyroid cancer staging determined?
Thyroid cancer, like most others, is staged based upon three criteria:
- T = how large the main tumor is when it is found
- N = the presence of cancer in lymph nodes and their location
- M = whether the cancer has spread or metastasized to other parts of the body. Thyroid cancer has been known to spread locally or to distant parts of the body including lungs and bone.
Staging from I to IV, including subgroups, is different for each type of cancer and helps predict outcome and survival. There are also different staging considerations for patients older or younger than age 45 for papillary and follicular thyroid cancers.
What kinds of specialists treat thyroid cancer?
A variety of physicians may be involved in the evaluation, diagnosis, and treatment of thyroid cancer. Primary care professionals may help coordinate care and may be the persons who make the initial diagnosis of thyroid gland abnormalities. Endocrinologists are specialists who specifically care for the thyroid. Surgeons may operate on the thyroid gland and thyroid cancer; these may be general surgeons or those with special training in head and neck surgery. Interventional radiologists may help with aspiration to obtain tissue samples, but this is also frequently performed by endocrinologists. Radiation oncologists, who are trained to provide radiation therapy treatments, may occasionally be asked to provide treatment. The care of thyroid cancer requires a team approach, but the members vary depending upon geographic location and availability of specialists.
Overview of Typical Thyroid Cancer Treatment
- Thyroid cancer is usually diagnosed by sticking a needle into a thyroid nodule or removal of a worrisome thyroid nodule by a surgeon.
- The thyroid nodule is looked at under a microscope by a pathologist who will then decide if the nodule is benign (95% to 99% of all nodules that are biopsied are benign) or malignant (less than 1% of all nodules, and about 1% to 5% of nodules that are biopsied).
- The pathologist decides the type of thyroid cancer: papillary, follicular, mixed papilofollicuar, medullary, or anaplastic.
- The entire thyroid is surgically removed; sometimes this is done during the same operation where the biopsy takes place. Your surgeon will assess the lymph nodes in the neck to see if they also need to be removed. In the case of anaplastic thyroid cancer, your doctor will help you decide about the possibility of a tracheostomy.
- About 4 to 6 weeks after the thyroid has been removed, you will undergo radioactive iodine treatment. This is very simple and consists of taking a single pill in a dose that has been calculated just for you. You will need avoid contact with other people for a couple of days so that others are not exposed to the radioactive materials.
- A week or 2 after the radioactive iodine treatment, you will have to start taking a thyroid hormone pill. No one can live without thyroid hormone, and if you don’t have a thyroid anymore, you will need to take levothyroxine (usually one pill a day) for the rest of your life. This is a very common medication (examples of brand names include Synthroid and Levoxyl).
- Every 6 to 12 months, you will visit your endocrinologist for blood tests to determine if the dose of daily thyroid hormone is correct and to make sure that the thyroid tumor did not return. The frequency of these follow-up tests will vary greatly from patient to patient. Endocrinologists are typically quite good at this and will typically be the type of doctor that you follow up with long-term.