What's in this article?
Systemic Lupus Erythematosus Overview
Systemic lupus erythematosus (SLE) is an autoimmune disease in which the body’s immune system mistakenly attacks healthy tissue. It can affect the skin, joints, kidneys, brain, and other organs.
Signs and Symptoms of Systemic Lupus Erythematosus
Systemic Lupus Erythematosus is a chronic autoimmune disease that can affect almost any organ system; thus, its presentation and course are highly variable, ranging from indolent to fulminant.
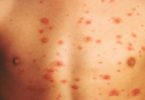
In childhood-onset Systemic Lupus Erythematosus, there are several clinical symptoms more commonly found than in adults, including malar rash, ulcers/mucocutaneous involvement, renal involvement, proteinuria, urinary cellular casts, seizures, thrombocytopenia, hemolytic anemia, fever, and lymphadenopathy.
In adults, Raynaud pleuritis and sicca are twice as common as in children and adolescents.
The classic presentation of a triad of fever, joint pain, and rash in a woman of childbearing age should prompt investigation into the diagnosis of Systemic Lupus Erythematosus.
Patients may present with any of the following manifestations :
- Constitutional (eg, fatigue, fever, arthralgia, weight changes)
- Musculoskeletal (eg, arthralgia, arthropathy, myalgia, frank arthritis, avascular necrosis)
- Dermatologic (eg, malar rash, photosensitivity, discoid lupus)
- Renal (eg, acute or chronic renal failure, acute nephritic disease)
- Neuropsychiatric (eg, seizure, psychosis)
- Pulmonary (eg, pleurisy, pleural effusion, pneumonitis, pulmonary hypertension, interstitial lung disease)
- Gastrointestinal (eg, nausea, dyspepsia, abdominal pain)
- Cardiac (eg, pericarditis, myocarditis)
- Hematologic (eg, cytopenias such as leukopenia, lymphopenia, anemia, or thrombocytopenia)
In patients with suggestive clinical findings, a family history of autoimmune disease should raise further suspicion of Systemic Lupus Erythematosus.
Causes of Systemic Lupus Erythematosus
The exact cause of Systemic Lupus Erythematosus is not known, but several factors have been associated with the disease.
- Genetics. The disease is not linked to a certain gene, but people with lupus often have family members with other autoimmune conditions.
- Environment. There may be environmental triggers like ultraviolet rays, certain medications, a virus, physical or emotional stress, and trauma.
- Gender and Hormones. Systemic Lupus Erythematosus affects more women than men. Women also experience worsening of symptoms during pregnancy and with their menstrual periods. Both of these observations have led some medical professionals to believe that the female hormone estrogen may play a role in causing Systemic Lupus Erythematosus. However, more research is still needed to prove this theory.
Treatment of Systemic Lupus Erythematosus
There is no cure for Systemic Lupus Erythematosus. The goal of treatment is to control symptoms. Severe symptoms that involve the heart, lungs, kidneys, and other organs often need treatment from specialists.
Mild forms of the disease may be treated with:
- NSAIDs for joint symptoms and pleurisy, after talking with your doctor
- Corticosteroid creams for skin rashes
- A drug also used to treat malaria (hydroxychloroquine) and low-dose corticosteroids for skin and arthritis symptoms
Treatments for more severe Systemic Lupus Erythematosus may include:
- High-dose corticosteroids
- Cytotoxic drugs (drugs that block cell growth or drugs which dampen or suppress the immune system): These medicines are used if you do not get better with corticosteroids, or if your symptoms get worse when you stop taking them. Side effects from these drugs can be severe, so you need to be monitored closely if you take them.
If you have Systemic Lupus Erythematosus, it is also important to:
- Wear protective clothing, sunglasses, and sunscreen when in the sun
- Get preventive heart care
- Stay up-to-date with immunizations
- Have tests to screen for thinning of the bones (osteoporosis)