What's in this article?
Streptococcus is a genus of spherical Gram-positive bacteria belonging to the phylum Firmicutes and the lactic acid bacteria group.
Streptococcal infection group A is also known as streptococcal disease. It is caused by a bacterium known as Group A (beta-haemolytic) Streptococcus. It can cause sore throat (pharyngitis), scarlet fever or serious complications in rare cases. Occasionally streptococcal infection group A can lead to serious complications such as rheumatic fever, which can affect the heart, and kidney disease (glomerulonephritis).
Strep is short for Streptococcus, a type of bacteria. There are two types: group A and group B.
 Group A strep
Group A strep
causes
- Strep throat – a sore, red throat, sometimes with white spots on the tonsils
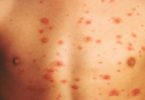
- Scarlet fever – an illness that follows strep throat. It causes a red rash on the body.
- Impetigo – a skin infection
- Toxic shock syndrome
- Cellulitis and necrotizing fasciitis (flesh-eating disease)
Group B strep
can cause blood infections, pneumonia and meningitis in newborns. A screening test during pregnancy can tell if you have it. If you do, I.V. antibiotics during labor can save your baby’s life. Adults can also get group B strep infections, especially if they are elderly or already have health problems. Strep B can cause urinary tract infections, blood infections, skin infections and pneumonia in adults.
Antibiotics are used to treat strep infections.
What is a GAS (Group A streptococcal) infection?
GAS is a bacterium commonly found on the surface of the skin and inside the throat.
These bacteria commonly cause mild throat, skin, ear and sinus infections in both adults and children. More rarely these bacteria cause an invasive infection where they penetrate deeper into the tissues and organs of the body causing more serious disease.
Examples of invasive disease caused by GAS are septicaemia (infection of the blood), pneumonia (infection of the lungs), puerperal sepsis (infection associated with childbirth), necrotising fasciitis (an infection of the deeper layers of skin more commonly known as flesh eating disease) and osteomyelitis (infection of the bone).
When GAS bacteria invade normally sterile parts of the body they can multiply rapidly and produce poisons. If the bacteria gain access to the deep layers of skin, the poisons produced can lead to destruction of the flesh and gangrene and it may be necessary for an individual to undergo surgery to remove the infection including amputation.
The inflammatory response of the body to poisons produced by GAS can lead to streptococcal toxic shock syndrome (STSS). STSS is a very serious condition with high rates of mortality (varying from 30 to 70%). During the course of STSS a patient develops problems with their circulatory system which in turn leads to organ damage. If left untreated STSS would be fatal.
In rare cases, GAS bacteria can cause meningitis if they gain access to the ‘meninges’ – the membranes that surround and protect your brain and spinal cord. The meninges are filled with a liquid called cerebrospinal fluid (CSF), which is there to bathe the brain and cushion it against physical damage when you hit your head.
Bacteria can multiply freely in CSF, and there they release poisons, causing inflammation and swelling in the meninges and the brain tissue itself. This increases pressure on the brain, producing symptoms of meningitis such as headache, stiff neck and dislike of bright lights. As the disease progresses, individuals become drowsy, confused, and delirious. They may have seizures and eventually lose consciousness.
How common is invasive infection by GAS?
Whilst mild illnesses caused by GAS are quite common, invasive infection is much rarer affecting approximately 3 people per in 100,000 in the UK.
Incidence of invasive infection due to GAS also fluctuates over time. Severe infections were uncommon in western Europe in the second half of the 20th century but increased during the mid-1980s in Great Britain. It has been speculated that the fluctuation in severity of infections over time may be attributable to natural fluctuation in the types of strains of bacteria in circulation (with some bacterial strains being more invasive than others).
Who gets invasive GAS infection?
Invasive GAS infection is usually isolated in nature (i.e it is very rare to have two cases of invasive disease occur together). However, the bacteria are transmitted from the throat or the skin. School children and those living in close proximity to others, for example in institutions, are more likely to carry and transmit GAS.
Almost one third of those who get invasive disease have no risk factors whatsoever. However, people with the following problems may be at increased risk of invasive infection by GAS because of breaks in the skin:
- Patients with a recent history of varicella infection (chicken pox)
- Patients who have undergone surgery
- Patients with traumatic injury
- Injecting drug users
Some patients may be at increased risk of infection because of a weakened immune system. For example:
- Patients who used nonsteroidal anti-inflammatory drugs (NSAIDs)
- Patients with HIV, diabetes, cancer, alcohol abuse
What is a GBS (Group B streptococcal) infection?
This form of meningitis is caused by Group B streptococcal (GBS) bacteria: Streptococcus agalactiae. GBS is the biggest cause of neonatal meningitis (meningitis in newborn babies) in the UK and Ireland, and can also cause septicaemia (blood poisoning) and pneumonia.
The bacteria normally live in the bowels and the vagina and sometimes in the back of the nose and throat. The bacteria can be transmitted from mother to baby before or during birth. An estimated 20 -30 %1 of pregnant women carry the bacteria but 99%1 of babies born to mothers who carry the bacteria are perfectly healthy.
A recent study, supported by the Foundation, found that the incidence of GBS infection in newborns in the UK and Ireland is around 7 cases per 10,000 live births (although this figure varies from country to country; 9 cases per 10,000 live births in Northern Ireland to 6 cases per live births in Ireland to 4 cases per 10,000 live births in Scotland).
There are two forms:
- early onset is normally septicaemia, causing shock and breathing difficulty and occurs at birth or within the first six2 days of life. The baby catches the bacteria from the birth canal during labour. Approximately 60 – 70 % of GBS infection is early onset.
- late onset is normally meningitis and causes fever, breathing difficulty, feeding problems and fits. It occurs in the first 7 – 902 days of life and is probably transmitted when babies are in contact with hands contaminated by the bacteria.
GBS pneumonia can be early or late in onset.
GBS disease can occur in mothers before or after giving birth but this is less common than in babies. Infection in adults is rare although studies in recent years have shown a slight increase3. People with immune problems are at a slightly increased risk from GBS infection.
Mothers of babies affected sometimes feel distressed that they may have been the source of infection. It is important to remember that GBS bacteria are just one of many types of bacteria which naturally live in our bodies, and most babies are not affected by them.
Although the bacteria can be passed on, a person with GBS infection does not pose a risk to others in the community.
Although most babies who get this disease survive with no severe problems, it is a serious illness. Nearly 10% of babies2 affected do not survive, and those who recover may have after effects such as deafness, brain damage and problems with movement and co-ordination. The fatality rate is higher in premature babies.
Antibiotics can be given to women during labour or to babies after birth to kill the bacteria. These women can be identified by bacteriological screening, involving taking swabs from the vagina and rectum, or by risk-factor based screening. Risk factors for GBS infection may include having a previous baby with GBS, premature delivery, prolonged rupture of membranes, or when the mother herself is feverish during delivery, or ill with GBS.
The study mentioned above contributed to UK guidelines developed by the Royal College of Obstetricians and Gynaecologists4. In Ireland each hospital has its own protocol on GBS, and these are generally similar to the RCOG guidelines. Screening for GBS is not routinely done in Ireland or the UK.
Immunisation of mothers could also prevent GBS, and several potential vaccines are in development.