What's in this article?
What is Strep
Group A Streptococcus is a bacterium that can cause a wide range of infections. Many People may also carry group A streptococci in the throat or on the skin and have no symptoms of illness. Most GAS infections are seriously mild illnesses such as “strep throat,” or impetigo (a skin infection).
How are group A streptococci spread?
These bacteria are spread through direct contact with mucus from the nose or throat of persons who are infected or through contact with infected wounds or sores on the top skin. Ill persons, such as those who have strep throat or skin infections, are the most to spread the infection. The persons who carry the bacteria but have no symptoms are much less contagious.
When Treating an infected person with an antibiotic for 24 hours or longer generally eliminates their ability to spread the bacteria. However, it is more important to complete the entire course of antibiotics as prescribed. It is not that household items like plates, toys, or cups spread these bacteria.
Group B streptococcus (GBS) is a type of bacterial infection that can be found in a pregnant woman’s vagina or rectum. This kind of bacteria is normally found in the vagina and/or rectum of about 25 % of all healthy, adult women. Those women who tested positively for GBS are said to be colonized.
How is group B strep transmitted?
In newborns, GBS infection is acquired through direct contact with the bacteria while in the uterus or during delivery; thus, the infection was transmitted from the colonized mother to her newborn. Approximately 50% of colonized mothers will pass the bacteria to their babies during pregnancy and vaginal delivery. However, but not all babies will be affected by the bacteria, and statistics show to us that about only one of every 100-200 babies born to a GBS-colonized mother will actually go on to develop GBS infection.
Group B strep infection is more likely common in African Americans than in whites.
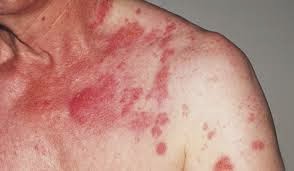
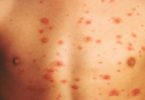
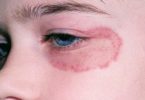
What is Rash
A rash is a change of the skin which affects its appearance, color, or texture. A rash may also be localized in one part of the body, or all the skin affect.
Rashes may cause the change of skin color, the itch, become warm, bumpy, chapped, dry, cracked or blistered, swell, and may be painful.
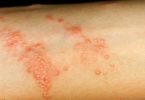
Symptoms, signs, and treatment of fungal infections
Fungal infections are fairly common but don’t appear nearly as often as rashes in the eczema category. Maybe the most common diagnostic mistake made by both patients and physicians is to almost automatically call scaly rashes “a fungus.” For instance, someone with several scaly spots on the arms,torso, or legs is much more likely to have a form of eczema or dermatitis than actual ringworm (the layman’s term for fungus). Likewise, yeasts may also botanically related to fungi and can cause skin rashes. These tend to affect folds of skin (like the skin under the breasts or the groin). They look like fiery red and have pustules around the edges. As is the case with ringworm, and many rashes that are no more than eczema or irritation get mislabeled “yeast infections.”
Fungus and yeast infections have little to do with hygiene , clean people can get infected also. Despite their reputation, fungal rashes are not commonly acquired from dogs or other animals. They are most easily acquired in showers, gym, locker rooms, or pools or from other family members. Treatment is usually very easy. Many effective antifungal creams can be bought at the drugstore without a prescription, including 1% clotrimazole (Lotrimin, Mycelex) and 1% terbinafine (Lamisil). In extensive cases, or when toenails are involved, a doctor prescription drug like oral terbinafine may be useful.
If a fungus has been repeatedly treated without success, you most likely considering the possibility that it was never really a fungus to begin with but rather a form of eczema. Eczema can be treated entirely differently from other fungal infections. A fungal infection can be independently confirmed by performing a variety of simple tests.