What's in this article?
Cryoglobulinemia Overview
The name literally means “cold antibody in the blood”, which refers to the chemical properties of the antibodies that cause this disease: cryoglobulins are antibodies that precipitate under cold conditions. Drug use is a prime risk factor for cryoglobulinemia because more than 90% of cases of cryoglobulinemic vasculitis are associated with hepatitis C infections. Hepatitis C is acquired by injection drug use (needle–sharing), tainted blood products, and (probably rarely), sexual transmission. Treatment of the underlying hepatitis may be an effective therapy for this type of vasculitis.
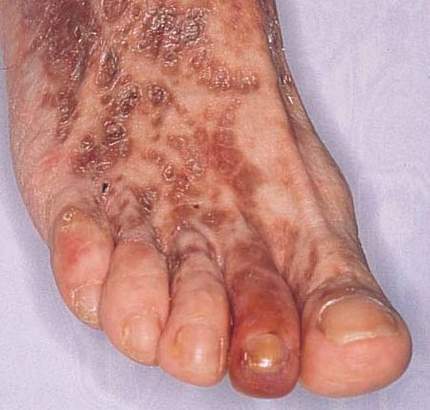
Pictured below is the hand from the same patient at different times. The image on the left is normal and the one on the right shows the patient in the midst of a flare of cryoglobuinemic vasculitis.
Who gets Cryoglobulinemia?
Most patients with cryoglobulinemia are chronically infected with hepatitis C virus (HCV). However, fewer than 3% of persons infected with HCV will develop cryoglobulinemic vasculitis, although the number of patients who test positive for cryoglobulins may be as high as 50%. Many of the remaining patients with cryoglobulinemia have lupus, Sjogren’s syndrome, rheumatoid arthritis, or white blood cell cancers (lymphoma, myeloma, or Waldenstrom’s macroglobulinemia) as the underlying cause. Development of cryoglobulinemia is rare among patients with these diseases. Since all of these diseases can affect persons of both sexes and all ages, cryoglobulinemia affects a similar diversity of patients.
Causes of Cryoglobulinemia
Cryoglobulins are antibodies. It is not yet known why they become solid or gel-like at low temperatures. When this occurs, these antibodies can block blood vessels. This may lead to problems ranging from skin rashes to kidney failure.
Cryoglobulinemia is part of a group of diseases that cause damage and inflammation of the blood vessels throughout the body (vasculitis). There are three main types of the disorder.
They are grouped based on the type of antibody that is produced:
- Cryoglobulinemia type I
- Cryoglobulinemia type II
- Cryoglobulinemia type III
Types II and III are also referred to as mixed cryoglobulinemia.
Type I cryoglobulinemia is most often related to cancer of the blood or immune systems.
Types II and III are most often found in people who have a chronic (long-lasting) inflammatory condition, such as an autoimmune disease or hepatitis C. Most people with mixed cryoglobulinemia have a chronic hepatitis C infection.
Other conditions that may be related to cryoglobulinemia include:
- Leukemia
- Multiple myeloma
- Mycoplasma pneumonia
- Primary macroglobulinemia
- Rheumatoid arthritis
- Systemic lupus erythematosus
Symptoms of Cryoglobulinemia
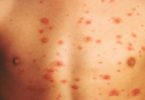
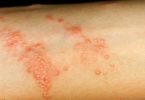
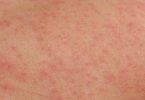
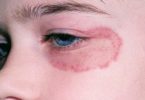
Most patients have weakness or fatigue, and many have sore joints or muscles. The most common appearance of vasculitis in the skin is purpura (bright red circles, from the size of a pinhead up to half an inch, often painful or itchy), but open sores are also common. Damage to nerves (neuropathy) causes numbness, tingling, severe burning pain, and or weakness in a hand or foot. Involvement of the gastrointestinal organs causes abdominal pain. Heart involvement could cause symptoms of a heart attack (chest pain) or congestive heart failure (difficulty breathing, swelling in the legs). Brain involvement can cause strokes, including multiple small strokes, and might also cause headache. Any symptoms that resolve within a few hours are unlikely to be caused by vasculitis. Kidney disease causes no symptoms until severe kidney failure occurs.
Treatment of Cryoglobulinemia
Mild or moderate forms of cryoglobulinemia can often be treated by taking steps to deal with the underlying cause.
- Mild cases can be treated by avoiding cold temperatures.
- Standard hepatitis C treatments usually work for patients who have hepetitis C and mild or moderate disease. The condition can return when treatment stops.
Severe cryoglobulinemia involves vital organs or large areas of skin. It is treated with corticosteroids and other medicines that calm the immune system.
Treatment may also involve plasmapheresis. In this procedure, blood plasma is taken out of blood circulation. It is replaced by fluid, protein, or donated plasma.