What's in this article?
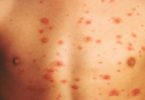
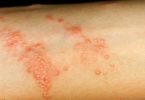
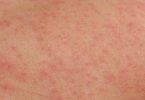
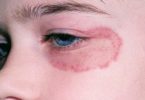
 Staphylococcal skin infections
Staphylococcal skin infections
Staphylococci (‘staph’) are a common type of bacteria that live on the skin and mucous membranes (eg. in nose) of humans. Staphylococcus aureus (S. aureus) is the most important of these bacteria in human diseases. Other staphylococci, including S. epidermidis, are considered commensals, or normal inhabitants of the skin surface.
About 15-40 per cent of healthy humans are carriers of S. aureus, that is, they have the bacteria on their skin without any active infection or disease (colonisation). The carrier sites are usually the nostrils and flexures, where the bacteria may be found intermittently or every time they are looked for.
What causes Staph. infections?
Despite being harmless in most individuals, S. aureus is capable of causing various infections of the skin and other organs. S. aureus infections are common in people with frequent skin injury, particularly if the skin is dry. Staph. skin infections are seen most commonly in pre-pubertal children and certain occupational groups such as healthcare workers. But they may occur for no obvious reason in otherwise healthy individuals.
Most staph. infections occur in normal individuals but underlying illness and certain skin diseases increase the risk of infection. These include:
♦ Severe atopic dermatitis
♦ Poorly controlled diabetes
♦ Kidney failure, especially those on dialysis
♦ Blood disorders such as leukaemia and lymphoma
♦ Malnutrition
♦ Low serum iron
♦ Alcoholism
♦ Intravenous drug users
♦ Medication with systemic steroids, retinoids, cytotoxics or immunosuppressives
♦ Immunoglobulin M deficiency
♦ Chronic granumomatous disease
♦ Chediak-Higashi syndrome
♦ Job’s and Wiskott Aldrich syndromes (associations of severe staphylococcal infection with eczema, raised immunoglobulin E and abnormal white cell function)
Staphylococcal aureus bacteria are classified as Gram-positive cocci based on their appearance under a microscope. They may occur singly or grouped in pairs, short chains or grape-like clusters. They are usually facultative anaerobes, that is, they are capable of surviving at various levels of oxygenation, and are generally very hardy organisms.
They are only able to invade via broken skin or mucous membranes, hence intact skin is an excellent human defence. Once they have invaded they have various ways to avoid host defences. They:
♦ Hide their antigens to avoid an immune response
♦ Kill infection-fighting cells (phagocytes)
♦ Survive within host infection-fighting cells.
♦ Develop resistance to antibiotics
♦ Release toxins (intoxication) these do not require the presence of live bacteria to have an effect.
Staphylococcal skin infections include:
♦ Impetigo (school sores)
♦ Ecthyma (crusted ulcers)
♦ Cellulitis (more often due to streptococcus)
♦ Hair follicle infections including staphylococcal folliculitis, boils (furuncles & carbuncles), abscess and sycosis (beard infection)
♦ Secondary skin infection of wounds, dermatitis, scabies, diabetic ulcers etc.
♦ Staphylococcal hypersensitivity reactions such as folliculitis decalvans (a cause of scarring hair loss)
Skin disease due to toxins produced by the bacteria include:
♦ Staphylococcal scalded skin syndrome (SSSS), which usually affects children less than five years old or rarely, adults with kidney failure.
♦ Toxic shock syndrome. This is a relatively uncommon illness usually resulting from the release of Toxic Shock Syndrome Toxin-1 (TSST-1) or enterotoxin B. These toxins are also known as superantigens as they are capable of generating a massive inflammatory response. Previous exposure makes a patient immune to these toxins i.e. they will not have a second attack.
♦ Staphylococcal scarlatina (scarlet fever).
Staphylococcal toxins can also cause food poisoning.
The diagnosis of staphylococcal skin infections should be confirmed by a positive laboratory culture of a swab from the infected site or blood culture.
In staphylococcal intoxications there may be no viable bacteria to culture and the diagnosis may be made retrospectively on the basis of a blood test demonstrating an immune response (seroconversion) to toxins following a compatible illness.
The treatment of staphylococcal infections includes:
♦ Appropriate antibiotics
♦ Drainage of pus collections
♦ Surgical removal (debridement) of dead tissue (necrosis)
♦ Removal of foreign bodies (eg. stitches) that may be a focus of persisting infection
♦ Treating the underlying skin disease (e.g. atopic eczema)
♦ Due to widespread antibiotic resistance, it is better to prevent staphylococcal infections where possible. The most effective way is to wash hands before touching broken skin.
It is also important to clear bacteria colonising the nostrils and under the fingernails with either antibiotic ointment (eg. fusidic acid or mupirocin) or petroleum jelly several times daily for one week of each month.
Antibiotic Resistance
Staphylococci are becoming increasingly resistant to many commonly used antibiotics including penicillins, macrolides such as erythromycin, tetracyclines and aminoglycosides.
Penicillin resistance in S. aureus is due to production of an enzyme called beta-lactamase or penicillinase. Methicillin (meticillin) and flucloxacillin are lactamase-resistant penicillins so are the antibiotics of choice in most staphylococcal skin infections. Unfortunately there is now increasing methicillin resistance (MRSA).
Penicillins with a beta-lactamase-inhibitor such as amoxicillin + clavulonic acid may be used to treat S. aureus infections and are sometimes effective against bacteria resistant to flucloxacillin. These antibiotics have a broad range of action against several bacteria and are best reserved for patients with mixed bacterial infections.
Patients who are allergic to penicillin are most reliably treated with vancomycin, although for minor infections macrolides such as erythromycin may be adequate. Macrolide resistance is also high among S. aureus but macrolides may be taken by mouth whereas vancomycin requires intravenous administration. Other options include clindamycin and rifampicin.