What's in this article?
Septicaemia is the presence of disease-causing bacteria in the blood. The human body is host to a range of different bacteria that live harmlessly in various places such as the mouth, skin, bowel and genital tract. However, these bacteria can cause disease if they get into the bloodstream, particularly if a person is unwell or if their immune system isn’t strong enough to keep the invading organisms under control.
This is why people with pre-existing medical conditions are most likely to get septicaemia. Severe infections, such as those of the lung, will also often give rise to septicaemia. Septicaemia is fatal in about one in four cases because of the effects of large numbers of multiplying bacteria and the toxins they release in the blood. The bacteria strains most commonly responsible include Escherichia coli(E. coli), Pneumococcus, Klebsiella, Pseudomonas, Staphylococcus and Streptococcus. Other terms for septicaemia include bacteraemia and blood poisoning.
Who gets meningitis and septicaemia?
Anyone of any age can get meningitis or septicaemia, but various factors can increase the risk.
- Geographical location – some countries have higher rates of meningitis and septicaemia than others. For example, many kinds of meningitis are much more common in developing countries than elsewhere. The only way to address this is through vaccination
- Environmental factors – exposure to smoke, for example, can make you more susceptible to infection
- Medical conditions and immunodeficiencies
- Age is one of the main risk factors.
What causes Septicaemia?
Septicaemia usually arises as a result of localised infection in the body. The primary site of infection may occur in the respiratory system, the skin, the gastrointestinal system or the genitourinary system. It may coincide with very aggressive infections such as meningitis.
Bacteria usually spill over from the primary infection site into the blood and are carried throughout the body thereby spreading infection to various systems of the body.
What are the signs and symptoms of septicaemia?
When septicaemia occurs, the immune system will immediately try to fight the infection in the bloodstream. This will bring on a number of sudden symptoms as the body fights the bacteria.
These might include:
- high temperature
- extreme tiredness
- violent shivering and chills
- faintness
- pale and clammy skin
- rapid and shallow breathing
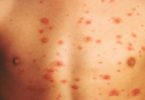
The skin may also develop pinprick bruises (called petechiae) or large purple areas (called purpura), which do not change colour if you roll a glass tumbler over them. This is a common sign of meningococcal septicaemia, a type of blood poisoning caused by the meningococcus bacteria, which can also cause meningitis.
In severe cases of blood poisoning the proteins and chemicals released in the blood to fight the bacteria can cause the blood vessels to become leaky and loss fluid such that the flow of blood is affected. When the flow of blood is affected this can lower blood pressure and ultimately cause damage to some of the organs like the brain and kidneys. This is called septic shock.
A healthy body fights septicaemia
Good health is the best defence against septicaemia. The immune system usually manages small-scale invasions of bacteria in the bloodstream so quickly that symptoms don’t even have a chance to develop. Tooth brushing, for example, can push mouth bacteria into the bloodstream via the gums and may cause a short-lived case of septicaemia. However, a person who has a pre-existing medical condition is at risk because their immune system is already taxed and may not have the strength to fight off the bacteria. Newborns and the very elderly are also at increased risk.
How is it diagnosed?
Septicaemia requires admission to an acute general hospital and may necessitate admission to an intensive care unit. The definitive test for diagnosing the condition is called a blood culture. This involves the taking of a small sample of blood and incubating it in the laboratory. If septicaemia is present bacteria will be detected and these can be studied further to establish which antibiotics will be effective against them.
Medical treatment may cause septicaemia
If a person has any type of medical treatment that requires invasive equipment, for example catheters, there is a risk that unfamiliar strains of bacteria may be introduced into their body. Examples of invasive treatments that can cause septicaemia include:
- Some dental treatments, such as drainage of an abscess.
- Surgery involving sites that naturally contain bacteria, such as the bowels.
- Long term placement of artificial parts, such as prosthetic joints.
- Bladder catheters, particularly if the person has urinary tract infections.
- Long term use of intravenous needles.
- Ostomy tubes, such as a colostomy (the bowel empties through a surgical hole in the abdominal wall instead of through the anus).
Can septicaemia be prevented?
There are few things you can do to prevent the risk of infection:
- To reduce the risk of wounds and burns becoming infected, keep them clean and properly dressed.
- Seek treatment for any mouth infections and boils.
- Keep up to date with the child’s immunisations. Immunisation can protect people from certain bacteria that can cause septicaemia. In the UK all babies are vaccinated against group C meningococcus and haemophilus as part of their immunisation programme.
- Ensure the child eats a healthy diet and exercises regularly in order to keep their immune system strong.