Porphyria refers to a group of rare inherited or acquired disorders of certain enzymes that normally participate in the production of porphyrins and heme. Porphyrins are essential for the function of hemoglobin a protein in your red blood cells that links to porphyrin, binds iron, and carries oxygen to your organs and tissue. Porphyria is not a single disease but a group of at least eight disorders that differ considerably from each other. A common feature in all porphyrias is the accumulation in the body of porphyrins or porphyrin precursors. Although these are normal body chemicals, they normally do not accumulate. Precisely which of these chemicals builds up depends on the type of porphyria.
Causes
Porphyria is most often an inherited mutation in one of the genes involved in heme production, although environmental factors can trigger symptoms in some cases.
Heme is a major component of hemoglobin, the protein in red blood cells that carries oxygen from your lungs to all parts of your body. Heme also plays a role in breaking down chemicals so they can be removed from your body. Heme is made mainly in the bone marrow and liver through the production of porphyrin and linkage with iron.
Eight different enzymes add and convert natural, smaller building blocks into porphyrin, which becomes heme with the addition of iron. Deficiency of a specific enzyme that’s involved in the body’s process for making heme can result in the buildup of porphyrins, causing symptoms. Each type of porphyria is due to the deficiency of a different enzyme.
Symptoms
Porphyrias involve three major symptoms:
- Abdominal pain or cramping (only in some forms of the disease)
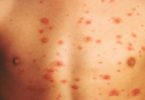
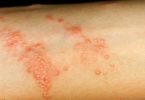
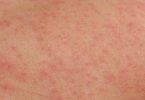
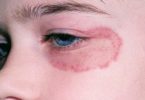
- Sensitivity to light that can cause rashes, blistering, and scarring of the skin (photodermatitis)
- Problems with the nervous system and muscles (seizures, mental disturbances, nerve damage)
Attacks can occur suddenly. They often start with severe abdominal pain followed by vomiting and constipation. Being out in the sun can cause pain, sensations of heat, blistering, and skin redness and swelling. Blisters heal slowly, often with scarring or skin color changes. The scarring may be disfiguring. Urine may turn red or brown after an attack.
Other symptoms may include:
- Muscle pain
- Muscle weakness or paralysis
- Numbness or tingling
- Pain in the arms or legs
- Pain in the back
- Personality changes
Attacks can sometimes be life threatening, producing:
- Low blood pressure
- Severe electrolyte imbalances
- Shock
Complications
Possible complications of porphyria include:
- Dehydration. Vomiting due to an attack of acute porphyria can lead to dehydration, which may require that you receive fluids through a vein (intravenously).
- Breathing difficulties. Acute porphyrias can cause muscle weakness and paralysis, which can cause breathing problems. If left untreated, they can also lead to respiratory failure.
- Low sodium in your blood. Called hyponatremia, this is usually linked to problems with sodium and water handling in your body.
- High blood pressure. Porphyrin buildup can damage your kidneys and may result in high blood pressure (hypertension).
- Chronic kidney failure. Porphyrin buildup may cause your kidneys to gradually lose their ability to function.
- Liver damage. Some forms of porphyria cause excessive porphyrins in your liver, which may lead to severe liver damage that can eventually require a liver transplant.
- Permanent skin damage. When your skin heals after cutaneous porphyria, it may have an abnormal appearance and coloring. Scars may remain on your skin as well, and lasting skin problems may cause your hair to fall out.
A health care provider diagnoses porphyria with blood, urine, and stool tests. These tests take place at a health care provider’s office or a commercial facility. A blood test involves drawing blood and sending the sample to a lab for analysis. For urine and stool tests, the patient collects a sample of urine or stool in a special container. A health care provider tests the samples in the office or sends them to a lab for analysis. High levels of porphyrins or porphyrin precursors in blood, urine, or stool indicate porphyria.
Sometimes multiple tests will be required before the diagnosis of a particular type of porphyria is possible. Because porphyria often runs in families, other family members can be tested and counseled after a positive diagnosis.
Treatment for porphyria depends on the type of porphyria the person has and the severity of the symptoms.
Acute porphyrias
Treatment of acute porphyrias focuses on providing rapid treatment of symptoms and preventing complications. This may require hospitalization in severe cases. Treatment may include:
- Stopping medications that may have triggered symptoms
- Medication to control pain, nausea and vomiting
- Prompt treatment of infections or other illness that may have caused symptoms
- Intravenous sugar (glucose) or sugar taken by mouth, if able, to maintain an adequate intake of carbohydrates
- Intravenous fluids to combat dehydration
- Injections of hemin, a medication that is a form of heme, to limit the body’s production of porphyrin
In rare instances, if symptoms are severe, a health care provider will recommend liver transplantation to treat acute porphyria. In liver transplantation, a surgeon removes a diseased or an injured liver and replaces it with a healthy, whole liver or a segment of a liver from another person, called a donor. A patient has liver transplantation surgery in a hospital under general anesthesia. Liver transplantation can cure liver failure.
Cutaneous Porphyrias
The most important step a person can take to treat a cutaneous porphyria is to avoid sunlight as much as possible. Other cutaneous porphyrias are treated as follows:
- Porphyria cutanea tarda. A health care provider treats porphyria cutanea tarda by removing factors that tend to activate the disease and by performing repeated therapeutic phlebotomies to reduce iron in the liver. Therapeutic phlebotomy is the removal of about a pint of blood from a vein in the arm. A technician performs the procedure at a blood donation center, such as a hospital, clinic, or bloodmobile. A patient does not require anesthesia. Another treatment approach is low-dose hydroxychloroquine tablets to reduce porphyrins in the liver.
- Erythropoietic protoporphyria. People with erythropoietic protoporphyria may be given beta-carotene or cysteine to improve sunlight tolerance, though these medications do not lower porphyrin levels. Experts recommend hepatitis A and B vaccines and avoiding alcohol to prevent protoporphyric liver failure. A health care provider may use liver transplantation or a combination of medications to treat people who develop liver failure. Unfortunately, liver transplantation does not correct the primary defect, which is the continuous overproduction of protoporphyria by bone marrow. Successful bone marrow transplantations may successfully cure erythropoietic protoporphyria. A health care provider only considers bone marrow transplantation if the disease is severe and leading to secondary liver disease.
- Congenital erythropoietic porphyria and hepatoerythropoietic porphyria. People with congenital erythropoietic porphyria or hepatoerythropoietic porphyria may need surgery to remove the spleen or blood transfusions to treat anemia. A surgeon removes the spleen in a hospital, and a patient receives general anesthesia. With a blood transfusion, a patient receives blood through an intravenous (IV) line inserted into a vein. A technician performs the procedure at a blood donation center, and a patient does not need anesthesia.
Porphyrias are life-long diseases with symptoms that come and go. Some forms of the disease cause more symptoms than others. Getting proper treatment and staying away from triggers can help lengthen the time between attacks.