What's in this article?
What is Psoriasis
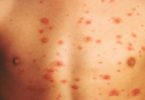
Psoriasis is a common skin condition that changes the life cycle of skin cells. Psoriasis causes cells to build up rapidly on the surface of the skin.
Psoriasis is a persistent, long-lasting (chronic) disease. There may be times when your psoriasis symptoms get better alternating with times your psoriasis worsens.
Experts believe that psoriasis occurs when the immune system overreacts, causing inflammation and flaking of skin. In some cases, psoriasis runs in families.
People with psoriasis often notice times when their skin gets worse. Things that can cause these flare-ups include a cold and dry climate, infections, stress, dry skin, and taking certain medicines.
Psoriasis facts
- Psoriasis is a chronic inflammatory skin disease.
- Patients with psoriasis who are obese are predisposed to diabetes and heart disease.
- Psoriasis can be initiated by certain environmental triggers.
- A predisposition for psoriasis is inherited in genes.
- Psoriasis is not contagious.
- Psoriasis gets better and worse spontaneously and can have periodic remissions (clear skin).
- Psoriasis is controllable with medication.
- Psoriasis is currently not curable.
- There are many promising therapies, including newer biologic drugs.
- Future research for psoriasis is promising.
Psoriasis Symptoms
Psoriasis signs and symptoms can vary from person to person but may include one or more of the following:
- Red patches of skin covered with silvery scales
- Small scaling spots (commonly seen in children)
- Dry, cracked skin that may bleed
- Itching, burning or soreness
- Thickened, pitted or ridged nails
Swollen and stiff jointsPsoriasis patches can range from a few spots of dandruff-like scaling to major eruptions that cover large areas.
Causes of Psoriasis
The exact cause remains unknown. There may be a combination of factors, including genetic predisposition and environmental factors. It is common for psoriasis to be found in members of the same family. The immune system is thought to play a major role. Despite research over the past 30 years looking at many triggers, the “master switch” that turns on psoriasis is still a mystery.
Psoriasis triggers
Psoriasis typically starts or worsens because of a trigger that you may be able to identify and avoid. Factors that may trigger psoriasis include:
- Infections, such as strep throat or skin infections
- Injury to the skin, such as a cut or scrape, bug bite, or a severe sunburn
- Stress
- Cold weather
- Smoking
- Heavy alcohol consumption
Certain medications including lithium, which is prescribed for bipolar disorder; high blood pressure medications such as beta blockers; antimalarial drugs; and iodides.
Can psoriasis affect my joints?
Yes, psoriasis is associated with joint problems in about 10%-35% of patients. In fact, sometimes joint pains may be the only sign of the disorder with completely clear skin. The joint disease associated with psoriasis is referred to as psoriatic arthritis. Patients may have inflammation of any joints (arthritis), although the joints of the hands, knees, and ankles tend to be most commonly affected. Psoriatic arthritis is an inflammatory, destructive form of arthritis and is treated with medications to stop the disease progression.
The average age for onset of psoriatic arthritis is 30-40 years of age. In most cases, the skin symptoms occur before the onset of the arthritis.