What's in this article?
What is Hidradenitis Suppurativa?
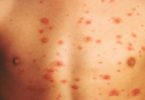
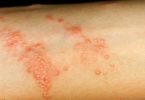
Hidradenitis suppurativa (HS) is a disease that usually begins as pimple-like bumps on the skin. The pimple-like bumps tend to develop in places that everyday pimples do not appear. Hidradenitis Suppurativa is most common on the underarms and groin.
Some people say that their Hidradenitis Suppurativa looks like one of these skin conditions:
- Pimples
- Deep-acne like cysts and blackheads
- Folliculitis (looks like swollen pimple with a hair in the center)
- Boils
Getting treatment for Hidradenitis Suppurativa is important. Early diagnosis and treatment can prevent Hidradenitis Suppurativa from worsening.
If Hidradenitis Suppurativa worsens, the pimple-like bumps can grow deep into the skin and become painful. They can rupture, leaking bloodstained pus onto clothing. This fluid often has a foul odor.
As the deep bumps heal, scars can form. Some people develop tunnel-like tracts under their skin. As the skin continues to heal and scar, the scars thicken. When thick scars form in the underarm, moving the arm can be difficult. Thick scars in the groin area can make walking difficult.
Because Hidradenitis Suppurativa can look lot like acne, folliculitis, or boils, it is best to see a dermatologist for a diagnosis. To a dermatologist’s trained eye, the differences between Hidradenitis Suppurativa and other skin diseases are subtle but obvious. Proper treatment depends on an accurate diagnosis.
Symptoms of Hidradenitis Suppurativa
Hidradenitis suppurativa commonly occurs around hair follicles with many oil and sweat glands, such as in the armpits, groin and anal area. It may also occur where skin rubs together, such as the inner thighs, under the breasts and between the buttocks. Hidradenitis suppurativa can affect one spot or multiple areas of the body.
Signs and symptoms of hidradenitis suppurativa include:
- Blackheads. Small pitted areas of skin containing blackheads — often appearing in pairs or a “double-barreled” pattern — are a common feature.
- Red, tender bumps. These bumps often enlarge, break open and drain pus. The drainage may have an odor. Itching and burning may accompany the bumps. They usually appear in areas where skin rubs against skin.
- Painful, pea-sized lumps. These hard lumps, which develop under the skin, may persist for years, enlarge and become inflamed.
- Tunnels. Over time, tracts connecting the lumps may form under the skin. These wounds heal very slowly, if at all, and can leak pus.
Hidradenitis suppurativa usually starts between puberty and age 40 with a single, painful bump that persists for weeks or months. For some people, the disease progressively worsens and affects multiple areas of their body. Other people experience only mild symptoms. Excess weight, stress, hormonal changes, heat or humidity can worsen symptoms. In women, the disease severity may lessen after menopause.
Causes of Hidradenitis Suppurativa?
The exact cause of hidradenitis suppurativa is unclear, but the lumps develop as a result of blocked hair follicles.
Smoking and obesity are both strongly associated with hidradenitis suppurativa, and if you’re obese and/or smoke it’s likely to make your symptoms worse.
Hidradenitis suppurativa usually starts around puberty, but it can occur at any age. It’s less common before puberty and after the menopause, which may suggest that the sex hormones play a part. Many people with the condition also have acne and hirsutism (excessive hair growth).
In rare cases, hidradenitis suppurativa may be linked to Crohn’s disease, particularly if it develops around the groin area and the skin near the anus. Crohn’s disease is a long-term condition that causes the lining of the digestive system to become inflamed.
Hidradenitis suppurativa runs in families in about a third of all cases. It’s not infectious and isn’t linked to poor hygiene.
Diagnosis for Hidradenitis Suppurativa
The diagnosis is primarily clinical, no pathognomonic test exists, and biopsy is rarely required, especially in well-developed lesions. The consensus approach indicates that three key elements are required to diagnose hidradenitis suppurativa: typical lesions, characteristic distribution, and recurrence. Arbitrarily, two recurrences over a period of 6 months have been used as a qualifier for a diagnosis. All three criteria must be present for the definitive diagnosis.
Treatment for Hidradenitis Suppurativa
There is no cure for hidradenitis suppurativa. But early and long-term treatment may help control pain, promote wound healing, keep new lumps from forming and prevent complications.
Several treatment options are available. Talk with your doctor about the risks and benefits of each and which combination of self-care, drugs or surgical procedures are right for you.
Medications
Your doctor might prescribe one or more of the following types of medications:
- Topical and oral drugs. These include antibiotics and drugs derived from vitamin A (retinoids).
- Other drugs that reduce inflammation. Injecting steroid medications directly into the tender nodule can reduce inflammation. Oral steroids, such as prednisone, can also help. But long-term use of prednisone has many side effects, including bone thinning (osteoporosis).
- Hormones. Small studies comparing oral antibiotics with hormonal therapy showed the hormonal therapy to be as effective as antibiotics in treating sores of hidradenitis suppurativa. Further study is needed. Hormonal therapy is not suitable for pregnant women due to the risk of side effects.
- Drugs that suppress the immune system. The drugs infliximab (Remicade) and adalimumab (Humira) show promise in the treatment of hidradenitis suppurativa. These “biologics” are TNF inhibitors. They work by neutralizing an immune system protein known as tumor necrosis factor (TNF). Researchers continue to assess these and similar drugs. Possible side effects include an increased risk of infection, heart failure and certain types of cancers.
- Pain medication. If over-the-counter pain relievers don’t help, your doctor may prescribe a stronger type. Examples include a fentanyl patch, codeine, morphine, gabapentin and pregabalin.
Surgery and other procedures
Hidradenitis suppurativa may be treated with various surgical approaches. The method used depends on the extent and location of the wounds, among other factors.
- Uncovering the tunnels. Known as unroofing, this procedure is gaining favor over incision and drainage. Your doctor cuts away the skin and flesh that cover any interconnected tunnels. This solution usually doesn’t have to be repeated.
- Punch debridement. This procedure is also called mini-unroofing and may be used to remove a single inflamed nodule.
- Incision and drainage. Surgical drainage may be an option when the disease involves a single small area. This treatment generally provides short-term pain relief, but the sores tend to recur.
- Tissue-sparing excision with electrosurgery. This may be an option for people with severe hidradenitis suppurativa. It combines skin-tissue-sparing excision with electrosurgical peeling (STEEP). The goal is to remove diseased tissue and preserve healthy tissue. You will be given general anesthesia for the STEEP procedure.
- Surgical removal. Surgical treatment of recurrent or severe symptoms involves removal of all involved skin. A skin graft may be necessary to close the wound. Even after you have surgery, sores may still occur in other areas. In men whose condition involves the area between the anus and scrotum, surgical removal of the scrotum is almost always necessary.
Alternative medicine
Zinc supplements taken daily may help reduce inflammation and prevent new outbreaks.