What's in this article?
What is Candida?
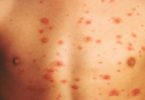
Candida is a strain of fungus that can cause an infection in your skin, among other locations. In normal conditions, your skin may host small amounts of this fungus, but problems arise when it begins to multiply and creates an overgrowth. More than 150 species of candida exist, but the majority of infections are caused by a species called Candida albicans.
The outlook for Candida infection is often very good. Generally, the condition isn’t serious and can be easily treated. However, uncontrolled infections can lead to potentially life-threatening problems especially in those with weakened immune systems. Quick treatment can help stop the spread of the fungus, while also improving (and potentially saving) your life.
What Causes Candida Infections?
There are many possible causes of candida including a diet high in sugar, refined carbohydrates and alcohol that help yeast to grow.
Potential Causes are as Follows:
Broad-Spectrum Antibiotics
Sometimes, antibiotics are needed to fight a stubborn infection to kill the offending bacteria in your system. The problem with antibiotics and with overusing them (often creating antibiotic resistance) is that they don’t just kill the bad bacteria; they kill the good ones, too.
The good bacteria in your system are responsible for digestion and keeping candida under control. After a long course (or multiple courses over a short period), antibiotics can make your body a literal breeding ground for candida.
Birth Control Pills
Unlike antibiotics, birth control pills in and of themselves do not directly cause a yeast infection or candida overgrowth syndrome. However, when a woman consumes a diet high in refined sugars and has had a course of antibiotics, birth control pills can adversely affect her body, leading to a candida infection.
Some women find that birth control pills seam to instigate yeast infections — and even long after the initial infection is gone, once they start taking the birth control pills again, candida can take root.
Oral Corticosteroids
Individuals that treat their asthma with corticosteroid inhalants are at an increased risk of developing candida in the mouth, leading to systemic candida overgrowth. It is imperative that individuals using corticosteroid inhalers for asthma follow the directions for swishing the mouth out after each use. If oral candidiasis is detected, can be treated with the gargling of coconut oil and a drop or two of essential clove oil.
Cancer Treatments
According to the Department of Clinical Research at Merck Research Laboratories, candidiasis can become invasive in cancer patients and prevent a serious complication. In this study, one-third of patients being treated for cancer had “invasive” candidiasis. Chemotherapy and radiation can both work to kill cancerous cells and tumors; however, they also kill off the healthy bacteria that naturally fight candida.
Diabetes
In a Type 1 or a Type 2 diabetic, sugar levels in the mouth and other mucous membranes are traditionally higher than in an individual without diabetes. Since candida is a type of yeast and sugar feeds yeast, it is understandable that those with diabetes are at a greater risk for developing candida overgrowth syndrome.
Weakened Immune System
Any individual with a weakened immune system is more likely to develop candida. This population includes infants, small children, the elderly, those diagnosed with HIV/AIDS, and other inflammatory and autoimmune conditions.
Predisposing factors for Candida Infection
- Infancy or old age
- Warm climate
- Occlusion e.g. plastic pants (babies), nylon pantyhose (women), dental plates
- Broad spectrum antibiotic treatment
- High-oestrogen contraceptive pill or pregnancy
- Diabetes mellitus, Cushing’s syndrome and other endocrine conditions
- Iron deficiency
- General debility e.g. from cancer or malnutrition
- Underlying skin disease e.g. psoriasis, lichen planus
- Immunodeficiency e.g. low levels of immunoglobulins, infection with human immunodeficiency virus (HIV)
- Chemotherapy or immunosuppressive medications such as systemic steroids
Treatment for Candida
Treatment for Candida skin infections is usually simple. You don’t need to be hospitalized unless you have problems with your immunity. Your doctor may prescribe drying agents or antifungal creams, ointments, or lotions to be applied to your skin.
You will most probably be prescribed over-the-counter drugs, such as ketoconazole or clotrimazole, both of which are from a class of antifungal drugs known as azoles. They don’t have serious side effects as compared to other antifungal agents like nystatin or amphotericin B. The infection should clear in about seven to 10 days.
If the infection persists or becomes more severe, your doctor may include some systemic antifungal medications (oral or injectable) in your therapy.