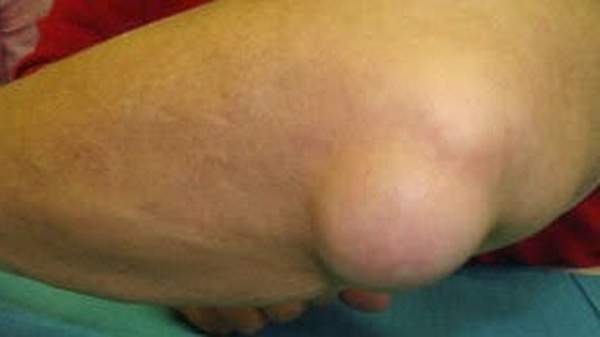
Bursitis is the inflammation of one or more bursae (small sacs) of synovial fluid in the body. The bursae is a sac filled with lubricating fluid, located between tissues such as bone, muscle, tendons, and skin, that decreases rubbing, friction, and irritation. The most common locations for bursitis
are in the shoulder, elbow and hip. But you can also have bursitis by your knee, heel and the base of your big toe. Bursitis often occurs near joints that perform frequent repetitive motion.
Causes
The most common causes of bursitis are repetitive motions, for example, repeated throwing of a ball, trauma like extensive kneeling, infection, and preexisting rheumatoid conditions.
Trauma
Trauma causes inflammatory bursitis from repetitive injury or direct impact.
- Chronic bursitis: The most common cause of chronic bursitis is minor trauma that may occur to the shoulder (subdeltoid) bursa from repetitive motion, for example, throwing a baseball. Another example is prepatellar bursitis (in front of the knee) from prolonged or repetitive kneeling on a hard surface to scrub a floor or lay carpet.
- Acute bursitis: A direct blow (let’s say you accidentally bang your knee into a table) can cause blood to leak into the bursa. This causes inflammation with pain as well as swelling.
Infections
Bursae close to the surface of the skin are the most likely to get infected with bacteria, a condition that is called septic bursitis. The most common bacteria to cause septic bursitis are Staphylococcus aureus or Staphylococcus epidermis. People with diabetes, alcoholism, certain kidney conditions, those with suppressed immune systems such as from cortisone medications (steroid treatments), and those with wounds to the skin over a bursa are at higher risk for septic bursitis. About 85% of septic bursitis occurs in men.
Rheumatoid Conditions
People with certain diseases such as gout and pseudogout can develop bursitis from crystal deposits. When these crystals form in a bursa, they cause inflammation leading to bursitis.
The main symptoms of bursitis are pain, swelling and tenderness in the affected area.
Any bursa can become inflamed, but bursitis most commonly occurs in the:
- shoulder
- elbow
- knee (known as housemaid’s knee)
- hip
Other areas affected can include the ankle, foot and Achilles tendon (the large tendon that attaches the heel bone to the calf muscle).
Doctors can often diagnose bursitis based on a medical history and physical exam.
If further testing is needed, you might undergo:
- Imaging tests. X-ray images can’t positively establish the diagnosis of bursitis, but they can help to exclude other causes of your discomfort. Ultrasound or MRI may be used if your bursitis can’t easily be diagnosed by a physical exam alone.
- Lab tests. Your doctor may perform blood tests or an analysis of fluid from the inflamed bursa to pinpoint the cause of your joint inflammation and pain.
Most cases of bursitis can be treated at home. Resting the affected area, using an ice pack (a frozen bag of vegetables wrapped in a tea towel works well) to reduce inflammation, and taking painkillers such as paracetamol and ibuprofen will help relieve your symptoms and speed up your recovery.
The pain usually improves within a few weeks, but the swelling may take longer to completely disappear.
See your GP if your symptoms do not improve after two weeks.
If your bursitis is not infectious, the doctor may inject the bursa with a corticosteroid to reduce inflammation.
If your bursitis is infectious, the bursa will be drained with a needle. The doctor will prescribe antibiotics to be taken in pill form. If the infection is very serious, does not respond to oral antibiotics, or if your immune system is weakened for another reason, you may be admitted to the hospital for IV antibiotics. Most causes of infectious bursitis, however, can be managed safely at home. Occasionally, a surgical operation to remove the bursa can be required.
The treatment for bursitis can be remembered with the following memory device:
P-R-I-C-E-M.
- Protection includes padding especially for bursae close to the surface of the skin on the ankles and knees.
- Relative rest of the affected area if possible may help symptoms. Choose alternate types of exercise activities that eliminate painful motions. Swimming may help rather than hurt.
- Ice is very effective in reducing inflammation and pain. Small ice packs, such as packages of frozen vegetables, applied to the area for 10 minutes at least twice a day may help decrease inflammation.
- Compression and Elevation are helpful when it is feasible to compress the area. An elastic bandage can be applied (especially to knees and elbows). Keep the area elevated above the heart to keep blood from pooling there.
- Medications such as aspirin or ibuprofen (Advil) can be helpful to reduce inflammation and pain. Consult your doctor before taking these if you are on any blood-thinning medications or have a history of stomach ulcers or kidney disease.
While not all types of bursitis can be prevented, you can reduce your risk and the severity of flare-ups by changing the way you perform certain tasks. Examples include:
- Using kneeling pads. Use some type of padding to reduce the pressure on your knees if your job or hobby requires a lot of kneeling.
- Lifting properly. Bend your knees when you lift. Failing to do so puts extra stress on the bursae in your hips.
- Wheeling heavy loads. Carrying heavy loads puts stress on the bursae in your shoulders. Use a dolly or a wheeled cart instead.
- Taking frequent breaks. Alternate repetitive tasks with rest or other activities.
- Walking around. Try not to sit in one position too long, especially on hard surfaces, because that puts pressure on the bursae in your hips and buttocks.
- Maintaining a healthy weight. Being overweight places more stress on your joints.
- Exercising. Strengthening your muscles can help protect your affected joint.
- Warming up and stretching before strenuous activities to protect your joints from injury.