What's in this article?
What is Osteomyelitis?
Osteomyelitis is an infection in a bone. Infections can reach a bone by traveling through the bloodstream or spreading from nearby tissue. Osteomyelitis can also begin in the bone itself if an injury exposes the bone to germs.
In children, osteomyelitis most commonly affects the long bones of the legs and upper arm, while adults are more likely to develop osteomyelitis in the bones that make up the spine (vertebrae). People who have diabetes may develop osteomyelitis in their feet if they have foot ulcers.
Once considered an incurable condition, osteomyelitis can be successfully treated today. Most people require surgery to remove parts of the bone that have died followed by strong antibiotics, often delivered intravenously, typically for at least six weeks.
Risks Of Osteomyelitis
There are a few conditions and circumstances that can increase your chances of osteomyelitis. Such as:
- diabetic disorders that affect blood supply to the bones.
- intravenous use of drugs.
- use of hemodialysis, a treatment used for kidney conditions.
- trauma to the tissue surrounding the bone.
- prosthesis or artificial limbs that introduce bacteria.
What are the types of bone infection?
Stages
Infection has several stages, from mild to severe.
Mild– Mild infection does not weaken the structural integrity of the bone and allows safe use of the bone for weight bearing.
Severe– Severe infection eats away at the structural integrity of the bone. When the bone loses its structural integrity, it cannot support weight and will likely break. This can be extremely painful.
Who Gets Osteomyelitis?
Only 2 out of every 10,000 people get osteomyelitis. The condition affects children and adults, although in different ways. Certain conditions and behaviors that weaken the immune system increase a person’s risk for osteomyelitis, including:
- Diabetes (most cases of osteomyelitis stem from diabetes)
- Sickle cell disease
- HIV or AIDS
- Rheumatoid arthritis
- Intravenous drug use
- Alcoholism
- Long-term use of steroids
- Hemodialysis
- Poor blood supply
- Recent injury
Bone surgery, including hip and knee replacements, also increase the chance of bone infection.
Osteomyelitis Causes
Bones, which usually are well protected from infection, can become infected through three routes:
- The bloodstream (which may carry an infection from another part of the body to the bones)
- Direct invasion (via open fractures, surgery, or objects that pierce the bone)
- Infections in nearby structures, such as natural or artificial joints or soft tissues
Injury, foreign bodies, and a decrease in the blood supply to organs or tissues (ischemia) may cause osteomyelitis. Osteomyelitis may form under deep pressure sores. Most osteomyelitis results from direct invasion or infections in nearby tissues.
When organisms that cause osteomyelitis spread through the bloodstream, infection usually occurs in the ends of leg and arm bones in children and in the spine (vertebrae) in adults, particularly older people. Infections of the vertebrae are referred to as vertebral osteomyelitis. People who are older, are debilitated (such as people living in nursing homes), have sickle cell disease, undergo kidney dialysis, and inject drugs using nonsterile needles are particularly susceptible to vertebral osteomyelitis.Staphylococcus aureus is the bacteria most commonly responsible for causing osteomyelitis that spreads via the bloodstream. Mycobacterium tuberculosis (the main cause of tuberculosis) and fungi can spread the same way.
Bacteria or fungal spores may also infect the bone directly through open fractures, during bone surgery, or from contaminated objects that pierce the bone.
Osteomyelitis may also occur where a piece of metal has been surgically attached to a bone, as is done to repair hip or other fractures. Also, bacteria or fungal spores may infect the bone to which an artificial joint is attached. The organisms may be carried into the area of bone surrounding the artificial joint during the operation in which the joint is installed, or the infection may occur later.
Osteomyelitis may also result from an infection in nearby soft tissue. The infection spreads to the bone after several days or weeks. This type of spread is particularly likely to occur in older people. Such an infection may start in an area damaged by an injury or surgery, radiation therapy, or cancer or in a skin ulcer (particularly a foot ulcer) caused by poor circulation or diabetes. A sinus, gum, or tooth infection may spread to the skull.
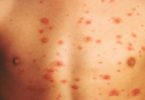
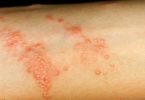
Osteomyelitis Symptoms
Signs and symptoms of osteomyelitis include:
- Fever or chills
- Irritability or lethargy in young children
- Pain in the area of the infection
- Swelling, warmth and redness over the area of the infection
Sometimes osteomyelitis causes no signs and symptoms or has signs and symptoms that are difficult to distinguish from other problems.
Osteomyelitis Diagnosed
If you have any symptoms of a bone infection your physician may use several methods to diagnose your condition. A physical exam is required to check for swelling, pain, and discoloration in the location of your complaint. Your doctor may order lab and diagnostic tests to determine the exact location and extent of the infection.
It is likely your doctor will order a blood test to check for the organisms causing the infection. Other tests to check for the bacteria are urine, fecal, and throat swabs.
A bone scan is diagnostic method that reveals cellular and metabolic activity in the bones. It uses a type of radioactive substance to highlight the bone tissue. If the bone scan does not provide enough information, you may need an MRI (magnetic resonance imaging). In some cases, a bone biopsy may even be necessary.
However, a simple bone X-ray may prove sufficient for your doctor to determine your plan of treatment.
Osteomyelitis Treatment
Figuring out if a person has osteomyelitis is the first step in treatment. It’s also surprisingly difficult. Doctors rely on X-rays, blood tests, MRI, and bone scans to get a picture of what’s going on. A bone biopsy is necessary to confirm a diagnosis of osteomyelitis. This also helps determine the type of organism, typically bacteria, causing the infection so the right medication can be prescribed.
For children and adults who have recently developed bone infections through the bloodstream, antibiotics are the most effective treatment. If the bacteria causing the infection cannot be identified, then antibiotics that are effective against Staphylococcus aureus and many types of bacteria (broad-spectrum antibiotics) are used. Depending on the severity of the infection, antibiotics may be given by vein (intravenously) for about 4 to 8 weeks but then may be given by mouth later. Some people have chronic osteomyelitis and need months of antibiotic treatment.