What's in this article?
What is Lyme Disease?
Lyme disease is caused by the bacterium Borrelia burgdorferi and is transmitted to humans through the bite of infected blacklegged ticks. Typical symptoms include fever, headache, fatigue, and a characteristic skin rash called erythema migrans. If left untreated, infection can spread to joints, the heart, and the nervous system. Lyme disease is diagnosed based on symptoms, physical findings (e.g., rash), and the possibility of exposure to infected ticks. Laboratory testing is helpful if used correctly and performed with validated methods. Most cases of Lyme disease can be treated successfully with a few weeks of antibiotics. Steps to prevent Lyme disease include using insect repellent, removing ticks promptly, applying pesticides, and reducing tick habitat. The ticks that transmit Lyme disease can occasionally transmit other tickborne diseases as well.
Lyme Disease facts
- Lyme disease is a bacterial illness that is spread by tick bites.
- Lyme disease can affect the skin, joints, heart, and the nervous system.
- Lyme disease occurs in phases, with the early phase beginning at the site of the tick bite with an expanding ring of redness.
- Lyme disease is diagnosed based on the patient’s clinical signs of illness and the detection of antibodies to the causative bacteria in the blood.
- Lyme disease is treated with antibiotics.
How Do People Get Lyme Disease?
Most people get Lyme from the bite of the nymphal, or immature, form of the tick. Nymphs are about the size of a poppy seed. Because they are so tiny and their bite is painless, many people do not even realize they have been bitten.
Once a tick has attached, if undisturbed it may feed for several days. The longer it stays attached, the more likely it will transmit the Lyme and other pathogens into your bloodstream.
If pregnant women are infected, they sometimes pass Lyme disease to their unborn children and, while not common, stillbirth has occurred. Some doctors believe other types of human-to-human transmission are possible but little is known for certain.
Symptoms of Lyme Disease
Early symptoms
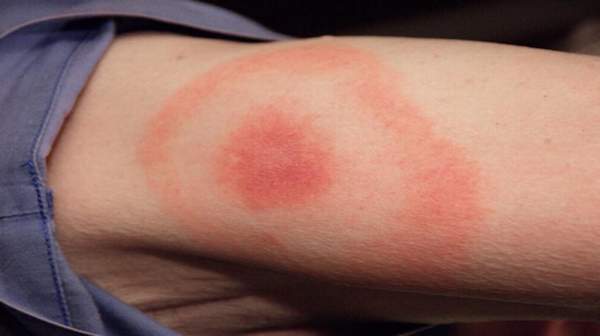
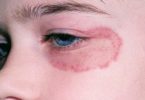
Many people with early-stage Lyme disease develop a distinctive circular rash at the site of the tick bite, usually around three to 30 days after being bitten. This is known as erythema migrans.
The rash is often described as looking like a bull’s-eye on a dart board. The affected area of skin will be red and the edges may feel slightly raised.
The size of the rash can vary significantly and it may expand over several days or weeks. Typically it’s around 15cm (6 inches) across, but it can be much larger or smaller than this. Some people may develop several rashes in different parts of their body.
However, around one in three people with Lyme disease won’t develop this rash.
Some people with Lyme disease also experience flu-like symptoms in the early stages, such as tiredness (fatigue), muscle pain, joint pain, headaches, a high temperature (fever), chills and neck stiffness.
Later symptoms
More serious symptoms may develop several weeks, months or even years later if Lyme disease is left untreated or is not treated early on. These can include:
- pain and swelling in the joints (inflammatory arthritis)
- problems affecting the nervous system – such as numbness and pain in your limbs, paralysis of your facial muscles, memory problems and difficulty concentrating
- heart problems – such as inflammation of the heart muscle (myocarditis) or sac surrounding the heart (pericarditis), heart block and heart failure
- inflammation of the membranes surrounding the brain and spinal cord (meningitis) – which can cause a severe headache, a stiff neck and increased sensitivity to light
Some of these problems will get better slowly with treatment, although they can persist if treatment is started late.
A few people with Lyme disease go on to develop long-term symptoms similar to those of fibromyalgia or chronic fatigue syndrome. This is known as post-infectious Lyme disease. It’s not clear exactly why this happens, but it’s likely to be related to overactivity of your immune system rather than persistent infection.
How is Lyme Disease Diagnosed?
Lyme disease may be difficult to diagnose because many of its symptoms mimic those of other disorders. Although a tick bite is an important clue for diagnosis, many patients cannot recall having been bitten by a tick. This is not surprising because the tick is tiny, and a tick bite is usually painless.
The easiest way for a doctor to diagnose Lyme disease is to see the unique bull’s-eye rash. If there is no visible rash (as is the case in about one-fourth of those infected), the doctor might order a blood test three to four weeks after the onset of the suspected infection to look for antibodies against the bacteria. Unfortunately, the Lyme disease bacterium itself is difficult to isolate or culture from body tissues or fluids. These blood tests are:
- ELISA. This blood test measures the levels of antibodies against the Lyme disease bacteria that are present in the body. Antibodies are molecules or small substances tailor-made by the immune system to lock onto and destroy specific microbial invaders.
- Western blot. This blood test identifies antibodies directed against a panel of proteins found on the Lyme bacteria. The test is ordered when the ELISA result is either positive or uncertain.
The presence of antibodies, however, does not prove that the bacterium is the cause of a patient’s symptoms. The presence of specific antibodies suggests a prior infection, which may or may not still be active.
Risk Factors for developing Lyme Disease
Lyme disease occurs most frequently in children 5-14 years of age and adults 40-50 years of age. The most substantial risk factor for Lyme disease is exposure to the ticks located in the high-risk areas of the country listed above, particularly in the New England states, as well as Minnesota and Wisconsin. Additional risk factors include recreational and occupational exposure to ticks and outdoor activities, including gardening, in woods and fields in the high-risk areas. No transplacental transmission (congenital infection) of Lyme disease from the mother to the unborn child has ever been described. Again, Lyme disease is not contagious from one person to another.
Treating Lyme disease
If you develop symptoms of Lyme disease, you will normally be given a course of antibiotic tablets, capsules or liquid. Most people will require a two- to four-week course, depending on the stage of the condition.
If you are prescribed antibiotics, it’s important you finish the course even if you are feeling better, because this will help ensure all the bacteria are killed.
If your symptoms are particularly severe, you may be referred to a specialist to have antibiotic injections (intravenous antibiotics).
Some of the antibiotics used to treat Lyme disease can make your skin more sensitive to sunlight. In these cases, you should avoid prolonged exposure to the sun and not use sunbeds until after you have finished the treatment.
There’s currently no clear consensus on the best treatment for post-infectious Lyme disease because the underlying cause is not yet clear. Be wary of internet sites offering alternative diagnostic tests and treatments that may not be supported by scientific evidence.
Preventing Lyme disease
There is currently no vaccine available to prevent Lyme disease. The best way to prevent the condition is to be aware of the risks when you visit areas where ticks are found and to take sensible precautions.
You can reduce the risk of infection by:
- keeping to footpaths and avoiding long grass when out walking
- wearing appropriate clothing in tick-infested areas (a long-sleeved shirt and trousers tucked into your socks)
- wearing light-coloured fabrics that may help you spot a tick on your clothes
- using insect repellent on exposed skin
- inspecting your skin for ticks, particularly at the end of the day, including your head, neck and skin folds (armpits, groin, and waistband) – remove any ticks you find promptly
- checking your children’s head and neck areas, including their scalp
- making sure ticks are not brought home on your clothes